Finding the right amount of this essential nutrient can feel confusing. You’re not alone if you’ve wondered about proper supplementation levels for yourself or your family.
The National Institutes of Health say this fat-soluble nutrient is rare in foods but crucial for bone health and immune function. Almost 20% of Americans have levels too low, making supplements key.
The 2024 Endocrine Society guidelines suggest vitamin d supplementation for certain groups. This includes children, pregnant individuals, adults over 75, and those with prediabetes. Cleveland Clinic research found about one-fifth of American adults take daily supplements, boosting a $1.1 billion industry in 2020.
Finding the right amount is tricky because it varies. Your age, body weight, skin tone, and health status all play a part.
This guide will help you understand recommendations from major health organizations. You’ll learn how to boost your intake through supplements, food, and safe sun exposure for better health.
Quick Answer
The recommended vitamin D dosage varies by age: 400 IU for infants, 600 IU for children and adults up to 70, and 800 IU for adults over 70 (NIH guidelines). However, many experts — including the Endocrine Society and Cleveland Clinic — recommend 1,000–2,000 IU daily for most adults to maintain optimal blood levels. Those treating a deficiency may need 4,000–5,000 IU daily under medical supervision. Always pair vitamin D with a meal containing fat for best absorption.
Key Takeaways
- Proper supplementation varies significantly by age, from newborns to seniors over 70
- The Endocrine Society recommends supplementation for children, pregnant people, adults over 75, and those with prediabetes
- Nearly 20% of Americans have inadequate levels, affecting bone health and immune function
- Individual factors like body weight and skin tone influence your personal requirements
- Evidence-based guidance from NIH and other major health organizations helps determine optimal daily amounts
- Combining supplements, fortified foods, and safe sun exposure provides the best approach
Understanding Vitamin D and Why Dosage Matters
To understand why the right vitamin D3 dosage is crucial, you need to know how it works in your body. Unlike other vitamins, Vitamin D: Benefits, Dosage, Food Sources and Deficiency Signs. It’s not just for strong bones; it also how vitamin D supports immune health in adults.
Getting the right amount is key to achieving optimal blood levels. Too little, and you miss out on important health benefits. Too much can cause problems, as we’ll discuss later.
What Vitamin D Does in Your Body
Vitamin D plays far more roles than most people realize. It’s not just for bones; it affects dozens of processes that keep you healthy.
The most known function is vitamin D’s role in calcium absorption in your gut. Without enough vitamin D, your body absorbs only 10-15% of calcium. But with enough, it absorbs 30-40%.
This calcium absorption is critical for maintaining proper blood calcium and phosphate levels. These minerals help keep your bones strong and prevent diseases like rickets and osteomalacia.
Vitamin D’s job goes beyond bones. Here are its key functions:
- Immune system regulation: Vitamin D helps your body fight infections better
- Inflammation reduction: It controls inflammation in your body
- Cell growth management: Vitamin D affects how cells grow and divide
- Neuromuscular function: Your muscles need it for proper contraction
- Glucose metabolism: It helps process blood sugar
- Mood regulation: Vitamin D affects neurotransmitters and mood
Understanding how vitamin D works helps explain why supplements are effective. When you get vitamin D from sunlight, food, or supplements, it’s not active right away. Your liver first converts it to 25-hydroxyvitamin D, or calcidiol.
This is the form measured in blood tests. Then your kidneys convert it into the active form: 1,25-dihydroxyvitamin D, or calcitriol. This hormone then binds to receptors in your body to do its work.
The Difference Between Vitamin D2 and D3
When shopping for supplements, you’ll find two main forms of vitamin D. Knowing the difference between vitamin d2 vs d3 is essential for choosing the right supplement.
Vitamin D2, or ergocalciferol, comes from plants. Manufacturers make it by exposing yeast or mushrooms to UV light. You’ll find D2 in some fortified foods and older supplements.
Vitamin D3, or cholecalciferol, comes from animals. Most supplements use D3 from lanolin (sheep’s wool). Vegan options use lichen, and your skin makes D3 when exposed to sunlight.
The question is: does it matter which form you take? Research shows it absolutely does.
| Factor | Vitamin D2 (Ergocalciferol) | Vitamin D3 (Cholecalciferol) |
|---|---|---|
| Source | Plant-based (UV-irradiated yeast/mushrooms) | Animal-based (lanolin) or lichen (vegan) |
| Potency | Lower effectiveness | 9.5 times more potent than D2 |
| Blood Level Increase | Raises 25(OH)D less effectively | Increases serum levels significantly more |
| Duration | Shorter-lasting in bloodstream | Maintains higher levels longer |
Cleveland Clinic research found that vitamin D3 is significantly superior to D2 for raising and maintaining blood levels. Studies showed D3 is 9.5 times more potent than D2 at increasing serum 25(OH)D concentrations.
Why is D3 so much better? Three main reasons explain its superiority:
- Better binding: D2 has a lower affinity for vitamin D binding protein, which transports the nutrient through your bloodstream
- Faster conversion: Your body converts D3 to 25(OH)D3 more quickly and efficiently than it converts D2 to 25(OH)D2
- Longer half-life: D3 stays in your system longer, providing sustained benefits between doses
This research shows why most doctors and nutritionists recommend D3 supplements over D2. D3 is better at vitamin d absorption and effectiveness, helping you reach and maintain optimal blood levels faster.
For anyone concerned about getting their vitamin d3 dosage right, choosing D3 over D2 is a simple way to ensure maximum benefit from your supplement. The form you take matters just as much as the amount.
Recommended Vitamin D Dosage: Official Guidelines
Ever felt confused by vitamin D supplement labels? You’re not alone. Different countries use different units, and health groups offer slightly different advice. Knowing the vitamin d daily dose recommendations helps you choose the right supplement.
Major health organizations have set official vitamin d requirements. These guidelines are based on years of research to prevent deficiency and support bone health. But first, you need to understand how vitamin D is measured.[1]
Understanding Measurement Units
Vitamin D dosage is shown in two main units: International Units (IU) and micrograms (mcg). This dual system can confuse many. But converting between them is easy once you know the formula.
One microgram equals 40 IU of vitamin D. So, 600 IU is 15 mcg, and 800 IU is 20 mcg. Most American supplements list IU, while European products use micrograms.
Here’s a quick conversion reference:
| Micrograms (mcg) | International Units (IU) | Common Use |
|---|---|---|
| 10 mcg | 400 IU | Infants, UK adult standard |
| 15 mcg | 600 IU | Children and adults up to 70 |
| 20 mcg | 800 IU | Adults over 70 |
| 25 mcg | 1,000 IU | Common supplement dose |
Knowing this conversion helps you compare different recommendations. Whether your doctor talks about micrograms or your supplement label shows IU, you’ll understand what you’re taking.
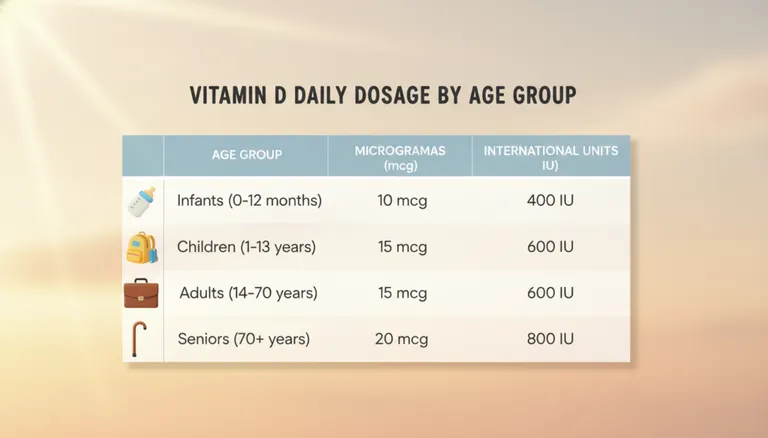
Daily Recommended Intake by Major Health Organizations
The National Institutes of Health (NIH) Food and Nutrition Board set the most followed RDA vitamin d guidelines in the U.S. These guidelines specify minimum amounts needed to maintain bone health and prevent deficiency across different life stages.
For infants aged 0-12 months, the NIH recommends 400 IU (10 mcg) daily. This applies whether babies are breastfed or formula-fed. Children and adults from ages 1 to 70 need 600 IU (15 mcg) daily. Adults over 70 require more, with recommendations increasing to 800 IU (20 mcg) daily.
Here’s a complete breakdown of official RDA vitamin d recommendations:
| Age Group | Daily Recommendation | IU | Micrograms (mcg) |
|---|---|---|---|
| Infants 0-12 months | Adequate Intake | 400 IU | 10 mcg |
| Children 1-18 years | RDA | 600 IU | 15 mcg |
| Adults 19-70 years | RDA | 600 IU | 15 mcg |
| Adults 71+ years | RDA | 800 IU | 20 mcg |
| Pregnancy & Lactation | RDA | 600 IU | 15 mcg |
The 2024 Endocrine Society guidelines suggest a more nuanced approach to vitamin d requirements. They recommend against supplementation beyond Institute of Medicine levels for healthy adults under 75 who get adequate sun exposure and dietary vitamin D.
However, the Endocrine Society identifies specific groups who benefit from higher doses:
- Children and adolescents: Higher doses help prevent rickets and reduce respiratory infections
- Adults 75 and older: Increased supplementation may lower mortality risk
- Pregnant individuals: Higher doses can reduce pre-eclampsia and preterm birth risks
- People with prediabetes: Adequate vitamin D may slow progression to diabetes
International guidelines vary somewhat from U.S. recommendations. The United Kingdom suggests 400 IU (10 mcg) daily for everyone aged 4 and up, particularly during fall and winter months. This reflects the UK’s limited sunlight during much of the year.
These variations don’t mean one organization is wrong and another right. Different recommendations reflect ongoing scientific debate about optimal vitamin D status versus merely adequate levels. The RDA focuses on preventing bone disease, while some researchers believe higher amounts support immune function, mood, and cardiovascular health.
It’s important to understand that these are minimum amounts for deficiency prevention. Your personal vitamin d daily dose might differ based on your health status, sun exposure, diet, and individual risk factors. Many healthcare providers recommend levels higher than the RDA for patients with specific health concerns or confirmed deficiency.
When choosing your supplementation strategy, use these guidelines as a foundation. They represent the consensus of expert panels reviewing thousands of studies. Your doctor can help determine whether you need the standard RDA or a personalized approach based on your unique circumstances.
Vitamin D Dosage for Infants and Babies
Babies grow fast in their first year, and vitamin D is key for this growth. Their bones are getting stronger every day. Without enough vitamin D, they could get rickets, a disease that’s now preventable with supplements.
The National Institutes of Health say all infants need 10 mcg (400 IU) daily from birth to 12 months. This amount helps keep their bones and immune system healthy. It’s important for all babies, no matter how they eat.[21]
Knowing about vitamin D for infants helps you make better choices for your baby’s diet. The good news is that supplements are easy, safe, and very effective.

Different Needs for Breast Milk and Formula
How your baby eats affects their vitamin D needs. It’s important to know this for their health.
Formula-fed babies get vitamin D from their formula. In the U.S., all formula is fortified with 40-100 IU of vitamin D per 100 calories. This means they get enough vitamin D from their formula alone.
Breastfed babies need extra vitamin D. Breast milk has very little vitamin D, even when the mother has enough. This means they only get a small part of their daily vitamin D from breast milk.
The American Academy of Pediatrics says all breastfed and partially breastfed infants should get 400 IU of vitamin D from the start. This should continue until they drink enough vitamin D-fortified formula or milk.
Partially breastfed babies also need extra vitamin D. If they don’t get enough from formula, adding drops ensures they get enough without too much.
Giving Supplements Safely to Newborns
It’s easy to give vitamin D drops to newborns once you know how. The drops come with a dropper that gives the right amount in just a few drops.
You can give the drops in different ways. Many parents put the drops in the baby’s mouth. Others mix them with breast milk or formula. Some put the drops on their nipple before breastfeeding.
When to give the drops is important. Vitamin D works best when given with food. This helps the baby’s body use it better.
Don’t worry about safety. 400 IU daily is safe for all babies. You can’t overdose at this dose, and missing a day won’t hurt them.
Some babies need more vitamin D. Premature babies and those with health issues might need more. Always talk to your pediatrician about your baby’s vitamin D needs.
Keep vitamin D drops in a cool, dry place. Store them away from sunlight and check the expiration date. Most drops stay good for 12-24 months when stored right.
Talk to your pediatrician about vitamin D for your baby. They can help with the right product and dosage. Most doctors recommend 400 IU daily for the first year, then adjust based on diet and sun.
Vitamin D supplements are a simple way to keep your baby healthy. This small step protects their bones, supports their immune system, and prevents rickets. With clear guidelines and safe products, making sure your baby gets enough vitamin D is easy.
Optimal Dosage for Children and Adolescents
From their first birthday to high school graduation, your child needs vitamin D for growth and health. These years are key for building strong bones. The foundation they establish now affects their bones for decades.
The National Institutes of Health say 600 IU (15 mcg) daily for all children ages 1-18. This amount prevents diseases like rickets. But, the Endocrine Society thinks many kids might need more to stay healthy and fight off infections.[1]
Knowing the right vitamin d for children dosage is important. It helps you make good choices for your family’s health. Let’s look at what your child needs at each stage.
Supporting Growth During the Early Years
Children ages 1-8 need 600 IU of vitamin D daily for their bones and teeth. Their bodies are always building new skeletal tissue. Vitamin D helps calcium get absorbed and used where it’s needed.
The safe maximum varies by age. Toddlers ages 1-3 can safely take up to 2,500 IU daily. For kids ages 4-8, it’s 3,000 IU daily.
It’s hard to get enough vitamin d for children from food alone. Here are some foods that help:
- Fortified milk: One cup has about 120 IU
- Fortified breakfast cereals: About 80 IU per serving
- Fortified orange juice: 100 IU per cup
- Eggs: 40 IU per yolk
- Salmon (3 ounces): 450 IU
Safe sun exposure also helps, but it depends on location and skin tone. About 10-15 minutes of midday summer sun can help. But, many kids spend a lot of time indoors, especially during school months.
Research shows that pediatric vitamin d supplements might help prevent colds and flu. This is especially true for kids who drink little milk, have darker skin, or live in northern climates with less sunlight.
Meeting Increased Needs During the Teen Years
Adolescents ages 9-18 also need 600 IU daily, but they might need more. Puberty brings rapid growth, and they’re building their final bone mass. This is a critical time for their bones.
The safe upper limit for teens is 4,000 IU daily. This gives more room for supplements when needed. Many teens don’t get enough vitamin D because of their lifestyle.
Several factors increase vitamin d for teens needs during adolescence:
- Increased screen time: Teens spend more hours indoors, reducing sun exposure
- Body composition changes: Obesity makes vitamin D harder to use
- Athletic demands: Young athletes need strong bones for intense training
- Darker skin tones: Higher melanin levels require longer sun exposure for vitamin D production
The Endocrine Society says kids and teens might need more vitamin D than the standard amount. This is especially true for preventing rickets and supporting their immune system.
Research also looks into vitamin D’s role in mood and mental health in teens. While more studies are needed, enough vitamin D might help with emotional well-being during these challenging years.
Getting children’s dosage right means finding ways that fit your family’s life. Chewable tablets and gummies are good options for kids. But, make sure they have enough vitamin D. Many kids’ multivitamins only have 400 IU, which might not be enough.
Parents often worry about safety, but the established upper limits are safe. A child taking 1,000 IU daily is well within safe ranges for all ages. The key is to be consistent, not perfect.
If your child doesn’t like supplements, focus on fortified foods and safe sun exposure. Even small amounts add up over time. If you’re worried about deficiency, especially if they have risk factors, consider getting their levels tested.
Supporting your child’s vitamin D status during these formative years is crucial. It sets them up for lifelong health benefits. Strong bones built now reduce fracture risk later, and optimal immune function keeps them healthier throughout childhood.
Adult Vitamin D Dosage Recommendations
Adults face a puzzling contradiction in vitamin D guidance. Official recommendations say one thing, while which vitamins are most important to take daily. The National Institutes of Health states that adults ages 19-70 need 600 IU (15 mcg) daily. This applies equally to men and women, including during pregnancy and lactation.[1]
However, many health experts believe this amount is too low for optimal wellness. Cleveland Clinic research shows that typical replacement requires at least 2,000 IU daily, with some researchers recommending 5,000 IU per day. The gap exists because official guidelines focus on preventing severe deficiency and maintaining bone health, not necessarily achieving optimal levels for other health benefits.
The 2024 Endocrine Society notes that healthy adults under 75 are unlikely to benefit from taking more than the RDA without specific risk factors. Yet individual needs vary dramatically based on lifestyle, body composition, and health status.

The 600 IU Standard for Ages 19-50
The official adult vitamin d dosage of 600 IU represents the minimum amount needed to maintain bone health in healthy individuals. This recommendation assumes you get some sun exposure and eat vitamin D-fortified foods.
Think of this amount as a safety net rather than an optimal target. It prevents rickets and osteomalacia—serious bone conditions caused by severe deficiency. But it may not address the vitamin’s role in immune function, mood regulation, or cardiovascular health.
For adults with minimal risk factors who spend time outdoors and maintain healthy body weight, 600 IU might suffice. Most people, however, have at least one factor that increases their needs beyond this baseline.
What Increases Your Vitamin D Requirements
Several factors can triple or quadruple your vitamin D needs compared to the standard recommendation. Understanding these helps you determine if you need more than the basic 600 IU.
Obesity tops the list of factors affecting vitamin d for adults. When your BMI exceeds 30, vitamin D gets sequestered in fat tissue. This means less circulates in your bloodstream where your body can use it. People with obesity often need 2-3 times the standard dose.
A fascinating predictive equation accounts for this reality:
Dose (IU) = 4,700 + [60 × (desired level in ng/mL – current level)] + 39 × BMI
For example, someone with a BMI of 32 wanting to raise their level from 20 ng/mL to 40 ng/mL would need approximately 5,900 IU daily. This mathematical approach provides personalized dosing rather than guessing.
Limited sun exposure dramatically reduces natural vitamin D production. Office workers, people living in northern states, and anyone who consistently wears sunscreen fall into this category. During winter months, even outdoor enthusiasts may not produce sufficient vitamin D from sunlight alone.
Darker skin pigmentation requires consideration too. Melanin reduces vitamin D synthesis in the skin. African American, Hispanic, and South Asian individuals may need 3-5 times longer sun exposure to produce the same amount as lighter-skinned people.
Certain medications interfere with vitamin D absorption or metabolism:
- Corticosteroids (prednisone, cortisone)
- Anti-seizure medications (phenytoin, phenobarbital)
- Weight-loss drugs that block fat absorption
- Cholesterol-lowering medications in some cases
Medical conditions affecting the digestive system present additional challenges. Crohn’s disease, celiac disease, and other malabsorption disorders prevent proper vitamin D uptake. Kidney disease impairs the conversion of vitamin D to its active form.
Special Considerations for Men and Women
While the official RDA remains identical for both sexes, vitamin d men and vitamin d women face unique situations that may require different approaches.
Women navigate several life stages with increased vitamin D demands. Pregnancy requires adequate levels for fetal skeletal development. The 600 IU minimum remains official guidance, though many obstetricians recommend higher amounts—typically 1,000-2,000 IU daily.
Lactation depletes maternal vitamin D stores as the nutrient passes into breast milk. Nursing mothers often need supplementation to maintain their own levels while providing for their babies.
Post-menopausal women face declining estrogen levels, which affects bone density. Sufficient vitamin D becomes crucial for calcium absorption and bone health during this transition. Many women over 50 benefit from 1,000-2,000 IU daily, especially with family history of osteoporosis.
Men have their own considerations regarding vitamin D status. Emerging research suggests connections between vitamin D and testosterone production, though studies continue. Prostate health may also relate to vitamin D levels, with some evidence pointing to protective effects.
The bottom line for vitamin d for adults? Consider your individual circumstances rather than blindly following the basic RDA. If you have obesity, limited sun exposure, darker skin, take certain medications, or have digestive conditions, you likely need more than 600 IU daily. However, if you’re a healthy adult without risk factors, the Endocrine Society suggests routine supplementation beyond the RDA isn’t necessary.
Working with your healthcare provider to assess your specific situation—and potentially test your blood levels—provides the most accurate guidance for your needs.
Vitamin D Requirements for Seniors Over 70
As we age, how vitamin D needs change through different life stages becomes crucial. This is especially true after 70. The body changes how it handles vitamin D, leading to specific needs for seniors. Knowing these needs is key to staying healthy and independent in our golden years.
The National Institutes of Health suggest 800 IU (20 mcg) daily for adults over 70. This is more than what younger adults need. It reflects the body’s changes with age.[1]
The 2024 Endocrine Society guidelines are even more detailed. They say people 75 and older might need more vitamin D to lower their risk of death.[4]

The Science Behind Increased Needs
Why does vitamin d for seniors become more important with age? It’s because your body works differently as you get older. These changes add up.
First, your skin doesn’t make vitamin D as well as it used to. A 70-year-old makes about 25% of the vitamin D a 20-year-old does from the same sun. This means seniors need more than just sun to get enough vitamin D.
Second, your kidneys don’t work as well with age. They turn vitamin D into its active form. So, even with supplements, you might not have enough active vitamin D.
Third, many seniors take medicines that affect vitamin D. Blood pressure meds, cholesterol drugs, and steroids are common culprits.
Having enough vitamin d over 70 is important for more than just bones. It helps prevent falls by keeping muscles strong and balance good. Falls are a big risk for older adults. Vitamin D also boosts the immune system, which gets weaker with age.
| Age Group | Standard Recommendation | Clinical Practice Range | Key Benefits |
|---|---|---|---|
| 19-50 years | 600 IU (15 mcg) daily | 1,000-2,000 IU daily | Bone maintenance, immune support |
| 51-70 years | 600 IU (15 mcg) daily | 1,000-2,000 IU daily | Bone health, muscle function |
| Over 70 years | 800 IU (20 mcg) daily | 2,000-5,000 IU daily | Fall prevention, fracture risk reduction, mortality reduction |
| Over 75 years | 800+ IU (20+ mcg) daily | 3,000-5,000 IU daily | Enhanced immune function, independence maintenance |
Overcoming Absorption Obstacles
Good news: aging doesn’t affect how well your gut absorbs vitamin D supplements. This means supplements work just as well for older adults as for younger ones.
But, getting enough vitamin D might require more than 800 IU. Cleveland Clinic research found that some seniors need 5,000 IU daily for adequate replacement. This shows that real-world experience with elderly vitamin d supplementation often requires higher doses.
Why might higher doses be needed? The reasons include less sun exposure, less efficient skin synthesis, possible kidney impairment, and medication interactions. Your doctor can test your blood levels and adjust your dose as needed.
Practical considerations are important for successful supplementation. Using daily pill organizers helps seniors remember to take their vitamins. Research shows daily dosing is better than weekly high doses for maintaining stable blood levels.
Take your vitamin D supplement with a meal that has some fat. Even a glass of whole milk or a handful of nuts will help. Fat improves absorption, making your supplement more effective.
Seniors with osteoporosis, a history of falls, or previous fractures should talk to their healthcare providers about higher-dose supplements. These conditions often need more aggressive vitamin D therapy, sometimes up to 5,000 IU daily.
The link between aging and vitamin d doesn’t have to be complicated. Simple daily supplementation at the right doses is a powerful tool for maintaining independence and quality of life. With regular testing and medical supervision, adequate vitamin D levels help seniors stay active, healthy, and independent for years to come.
Vitamin D Dosage by Health Goal
Your vitamin D needs change based on your health goals. While the usual amounts prevent deficiency, research shows different amounts can help with specific health issues. Knowing these targets helps you and your doctor create a plan just for you.[3]
Vitamin D isn’t a magic solution. It works best as part of a complete health plan. This includes eating right, exercising, and getting medical care when needed.

Supporting Strong Bones and Preventing Osteoporosis
Vitamin D for bones is key with calcium to keep bones strong. The NIH says vitamin D and calcium help older adults avoid osteoporosis and reduce fracture risk.[9]
While 600-800 IU daily prevents rickets and osteomalacia, more is needed for bone health. Studies show 800-1,000 IU daily with enough calcium (1,000-1,200 mg daily) helps prevent fractures in older adults.
For those with osteoporosis or osteopenia, doctors often prescribe more. They might give 1,000-2,000 IU daily, sometimes more based on blood tests.
Remember, calcium and vitamin D must work together. Taking vitamin D alone won’t fully protect your bones without enough calcium.
Strengthening Your Immune Defenses
The link between vitamin D immune system function is deeper than many think. Vitamin D receptors are in your immune cells, playing key roles in both innate and adaptive immunity.
Cleveland Clinic research shows vitamin D’s immunomodulatory and antiviral effects. They found that enough vitamin D might lower the risk and severity of infections, including respiratory illnesses and COVID-19.
Vitamin D modulates immune function and demonstrates significant biological effects on innate and adaptive immune systems, with immunomodulatory and antiviral properties that may help protect against infections.[13]
While the basic RDA prevents severe deficiency, some immunologists suggest higher levels for better immune function. Experts recommend keeping serum 25(OH)D levels between 40-60 ng/mL, which is higher than the standard 20 ng/mL threshold.
To reach these levels, many need 2,000-4,000 IU daily, though needs vary. This topic is still debated, so talk to your doctor before increasing your dose a lot.
Managing Mood and Seasonal Blues
Brain areas that control mood have vitamin D receptors, linking this nutrient to mental health. Research links deficiency to seasonal affective disorder (SAD) and depression, making vitamin D for depression an area of growing interest.
The evidence is mixed. Some studies show supplementation can reduce depression symptoms, especially in winter. Other research hasn’t found consistent benefits.
Studies on mood support have used doses from 1,000-4,000 IU daily. Results vary, suggesting vitamin D might help some more than others.
If you get winter blues or depression, ask your doctor about vitamin D testing. Fixing a deficiency might improve your mood, but it’s not a cure for serious depression. Always seek professional help for serious mood disorders.
Cardiovascular Protection and Blood Pressure
The connection between vitamin D heart health and heart function is promising in studies but needs careful interpretation. People with low vitamin D levels face higher heart disease and hypertension risks in population studies.
However, trials testing if supplementation prevents heart disease have mixed results. This difference between observational and experimental evidence is important.
The Endocrine Society doesn’t recommend high-dose vitamin D for heart health in people without deficiency. Still, keeping blood levels of at least 20 ng/mL, preferably 30-40 ng/mL supports overall health and may help heart health.
Most adults can reach these levels with 1,000-2,000 IU daily supplements. For heart benefits, focus on proven strategies like healthy eating, regular exercise, stress management, and any medications your doctor prescribes.
Work with your healthcare provider to see if higher vitamin D doses are right for you. Blood tests are key to knowing your current status and what you need.
Dosage for Vitamin D Deficiency Treatment
Discovering you have vitamin D deficiency doesn’t mean you’re stuck with it. You can correct low levels with the right dosing strategy. Vitamin D deficiency treatment needs a different approach than standard supplementation. It uses higher doses initially to rebuild your body’s depleted stores.
The treatment protocols help you work with your healthcare provider to restore healthy levels. This is crucial for your health.
The vitamin d deficiency dosage typically follows a two-phase approach. First, there’s an aggressive loading phase to quickly raise levels. Then, there’s ongoing maintenance to keep them steady. This strategy addresses both the immediate problem and the long-term need for adequate vitamin D.
Understanding Your Deficiency Level
Vitamin D deficiency is identified through a simple blood test. This test measures 25-hydroxyvitamin D, or 25(OH)D. Your doctor might order this test if you have risk factors like limited sun exposure, dark skin, obesity, or symptoms such as bone pain, muscle weakness, or unexplained fatigue.
The results reveal exactly where your levels stand. Health organizations define deficiency ranges slightly differently. But there’s general consensus on the categories.
The NIH defines deficiency as levels below 30 nmol/L (12 ng/mL). Inadequacy is at 30-50 nmol/L (12-20 ng/mL). Sufficiency is at 50+ nmol/L (20+ ng/mL). The Endocrine Society guidelines from 2011 set the deficiency threshold at less than 20 ng/mL. They also established minimum replacement dosage recommendations.
| Vitamin D Status | Blood Level (ng/mL) | Blood Level (nmol/L) | Health Implications |
|---|---|---|---|
| Severe Deficiency | Below 12 | Below 30 | Risk of rickets or osteomalacia |
| Deficiency | 12-20 | 30-50 | Increased bone loss, weakness |
| Insufficiency | 20-30 | 50-75 | Suboptimal bone health |
| Sufficiency | 30-50 | 75-125 | Adequate for most functions |
| Optimal (some experts) | 40-60 | 100-150 | Preferred for overall health |
Some experts prefer higher targets. They recommend levels of 40+ ng/mL for optimal health benefits beyond just bone health. Your healthcare provider will interpret your specific results. They will determine the appropriate vitamin d deficiency treatment based on your level and individual circumstances.
Loading Doses vs Maintenance Doses
When you’re deficient, you need higher doses initially. This is like filling an empty tank versus topping off a full one. This is where loading dose vitamin d protocols come into play. The loading phase uses substantially higher doses than standard supplementation to quickly correct the deficiency.
Common loading protocols include 50,000 IU once weekly for 8 to 12 weeks. This is a standard approach that many physicians prescribe. An alternative protocol uses 5,000 to 10,000 IU daily for 8 weeks. This provides similar total dosing but spreads it throughout the week. Both approaches effectively raise levels, though weekly high-dose therapy offers convenience with just one pill per week.
Cleveland Clinic research indicates that 5,000 IU daily is usually needed to correct deficiency. This highlights that restoration requires doses well above the standard RDA. The relationship between intake and blood level isn’t linear. How much your levels rise depends on your baseline level, body weight, absorption efficiency, and supplementation duration.
After the loading phase comes maintenance dosing to keep levels adequate long-term. Cleveland Clinic findings show that typical maintenance requires at least 2,000 IU daily. This is significantly more than the 600-800 IU RDA. People with risk factors like obesity, limited sun exposure, or darker skin often need 3,000 to 4,000 IU daily for maintenance.
Here’s a practical example: Someone with an initial level of 15 ng/mL might take 50,000 IU once weekly for 8 weeks. After completing this loading phase, they’d retest to confirm their level has risen to 30+ ng/mL. Once sufficiency is confirmed, they’d switch to 2,000 to 4,000 IU daily to maintain healthy levels.
Timeline for Correcting Deficiency
Most people wonder how long it takes to fix low vitamin D levels. The typical timeline for correcting vitamin d deficiency runs 8 to 12 weeks with appropriate loading doses. However, response varies significantly between individuals based on several factors including body weight, absorption capacity, and how deficient you were initially.
Some people reach sufficiency in 6 to 8 weeks, while others need 12 weeks or longer. This variation is why retesting after the loading phase is essential. It confirms whether your levels have normalized or if you need additional treatment. Your healthcare provider will typically recheck your 25(OH)D level about 8 to 12 weeks after starting treatment.
An important reality to understand: correcting deficiency isn’t a one-time fix. Most people need ongoing supplementation because the factors that caused deficiency usually persist. Unless your life changes dramatically, such as moving to a sunny climate and spending considerable time outdoors safely, you’ll likely need continued supplementation.
Many patients ask, “Can I ever stop taking it?” The honest answer is usually no, not without lifestyle changes that dramatically increase natural vitamin D production. Think of it like brushing your teeth—it’s an ongoing health practice, not a temporary intervention. The good news is that maintenance doses are lower than loading doses and easily incorporated into your daily routine.
Working with your healthcare provider ensures a personalized vitamin d deficiency dosage plan tailored to your specific needs. This includes appropriate testing before treatment, monitoring during the loading phase if needed, and retesting after treatment to confirm success. With the right strategy, deficiency is highly correctable, typically within a few months. Maintaining healthy levels long-term becomes straightforward with daily supplementation.
Testing Your Vitamin D Levels
Knowing when and how to test your vitamin D levels can help you make better choices about supplements. A vitamin d blood test checks your 25-hydroxyvitamin D, or 25(OH)D. This is the vitamin D stored in your blood.[16]
Your 25(OH)D levels show your total vitamin D from sunlight, food, and supplements. This test is the best way to check your vitamin D levels because it lasts 15 days in your blood.
This test is different from checking calcitriol, the active form of vitamin D. Doctors don’t use calcitriol for routine tests because it doesn’t show your vitamin D status well.
Knowing When Testing Makes Sense
The 2024 Endocrine Society guidelines say you shouldn’t get routine vitamin d tests unless you need to. This includes people with dark skin or obesity, even if they’re at higher risk for deficiency.[4]
They don’t recommend testing for everyone because we don’t know how vitamin d levels affect health in most people. Testing isn’t proven to be beneficial for most healthy individuals.
However, doctors might suggest testing in certain situations. You might need a vitamin d blood test if you have:
- Confirmed deficiency symptoms like bone pain, muscle weakness, or frequent infections
- Osteoporosis or a history of fractures
- Malabsorption conditions such as Crohn’s disease, celiac disease, or bariatric surgery
- Chronic kidney or liver disease affecting vitamin D metabolism
- Medications that interfere with vitamin D, including anticonvulsants or steroids
Testing is also a good idea before starting high-dose supplements and after treating deficiency. It helps confirm if your treatment worked.
Getting a vitamin d blood test is simple. It involves a blood draw, and you usually don’t need to fast. The test is relatively cheap and often covered by insurance. You’ll get your results in a few days.
Making Sense of Your Results
Your test results will show your 25(OH)D levels in ng/mL or nmol/L. Different labs use different units, which can be confusing.
The conversion is simple: 1 ng/mL equals 2.5 nmol/L, and 1 nmol/L equals 0.4 ng/mL. Most American labs report in ng/mL, while international labs often use nmol/L.
Here’s how to understand your vitamin d blood levels:
| Level (ng/mL) | Level (nmol/L) | Status | Health Implications |
|---|---|---|---|
| Below 12 | Below 30 | Severe Deficiency | High risk of rickets in children, osteomalacia in adults, increased fracture risk |
| 12-20 | 30-50 | Deficiency | Inadequate for bone health, may cause bone loss and weakness |
| 20-30 | 50-75 | Insufficiency | Adequate for basic bone health but possibly suboptimal for other functions |
| 30-50 | 75-125 | Sufficiency | Target range recommended by most experts for overall health |
| 50-80 | 125-200 | High-Normal | Generally safe, potentially beneficial for some conditions |
| Above 100 | Above 250 | Concerning | Risk of toxicity symptoms including hypercalcemia |
The NIH says levels below 30 nmol/L (12 ng/mL) show deficiency. Levels between 30-50 nmol/L (12-20 ng/mL) are generally inadequate for bone health. Levels above 50 nmol/L (20 ng/mL) are considered sufficient.
However, levels above 125 nmol/L (50 ng/mL) can be associated with adverse effects. This is where monitoring becomes important.
The Debate: Sufficient or Optimal?
The official “sufficient” threshold is 20 ng/mL. This level is enough to prevent bone diseases like rickets and osteomalacia.
But some researchers think we should aim for higher levels. They suggest keeping 25(OH)D levels between 30-40 ng/mL or even 40-60 ng/mL for better immune function, cancer prevention, and other benefits.
The conservative view says 20+ ng/mL is enough based on solid bone health evidence. We lack proof that higher levels provide additional benefits for other health outcomes. This is the position of most official health organizations.
The optimization view suggests levels of 40-60 ng/mL may offer benefits beyond bone health. These include enhanced immune response, better mood regulation, and cardiovascular protection. The Cleveland Clinic recommends maintaining 40-60 ng/mL specifically for immune support.
The risk of maintaining higher levels (30-60 ng/mL) is minimal when achieved through appropriate supplementation. These levels remain well below the toxicity threshold of 100+ ng/mL.
Your ideal target depends on your individual health goals and risk factors. Someone with osteoporosis might aim for the higher end of the range. A healthy young adult might be fine at 30 ng/mL.
The good news? You don’t always need testing to maintain healthy levels. Many people can safely take 1,000-2,000 IU daily without testing. This dosage stays well below toxicity risk while likely achieving adequate vitamin d blood levels.
If you do choose to test, discuss your results with your healthcare provider. They can help you understand your numbers in the context of your overall health. Together, you can decide if your current levels support your health goals or if adjustments are needed.
Maximum Safe Dosage and Toxicity Concerns
Vitamin D safety is good news. Vitamin d toxicity is rare and usually preventable. Your body handles vitamin D from sunlight and food well.[10]
Most toxicity cases come from too much supplement use. Knowing the safe limits helps you avoid too much vitamin d risks.
Safe Upper Intake Levels for Every Life Stage
The National Institutes of Health set safe daily vitamin D amounts. These are the highest amounts unlikely to harm most people. The vitamin d upper limit is a safety cap, not a recommended dose.[2]
The upper limit is your safety buffer. For adults, the 4,000 IU daily limit is much higher than the basic need. This means most people can safely take supplements without danger.
| Age Group | Upper Limit (IU/day) | Safety Margin vs RDA |
|---|---|---|
| Infants 0-6 months | 1,000 IU | 2.5x higher than RDA |
| Infants 6-12 months | 1,500 IU | 3.75x higher than RDA |
| Children 1-3 years | 2,500 IU | 4.2x higher than RDA |
| Children 4-8 years | 3,000 IU | 5x higher than RDA |
| Ages 9+ through adulthood | 4,000 IU | 5-6x higher than RDA |
Many experts say 4,000 IU daily is safe for adults. But, doses over 10,000 IU daily can be risky. Blood levels above 125 nmol/L (50 ng/mL) can cause problems, especially over 150 nmol/L (60 ng/mL).
Recognizing the Warning Signs of Excessive Intake
Vitamin d toxicity is rare and usually avoidable. It’s caused by too much calcium in the blood, not vitamin D itself. High vitamin D levels make your body absorb too much calcium.
The signs of too much vitamin d start with early symptoms. These include:
- Nausea and vomiting
- Weakness and fatigue
- Frequent urination and excessive thirst
- Loss of appetite
Moderate symptoms include bone pain, kidney problems, and heart rhythm issues. Severe cases can lead to confusion, kidney stones, and heart problems.
A case from Cleveland Clinic shows the seriousness and reversibility of toxicity. An 80-year-old man took 50,000 IU weekly instead of daily. This caused his vitamin D levels to soar, leading to high calcium and serious symptoms.
His symptoms, including confusion and difficulty speaking, went away after stopping the supplement and treating his calcium levels.
This case highlights the dangers of accidental overdosing. Mistaking weekly doses for daily, manufacturing errors, or taking too many supplements can lead to toxicity.
To stay safe, follow these tips:
- Keep supplements organized and labeled
- Tell your doctor about all supplements
- Don’t megadose without medical advice
- Seek help if you have concerning symptoms
The Sun Exposure Safety Question
Can you get too much vitamin d from the sun? No, you can’t. Sunlight doesn’t lead to vitamin d toxicity.
Your body has a built-in system to prevent too much vitamin D. It stops producing more after a certain point. This natural limit protects you from toxicity.
While sun exposure is safe for vitamin D, it’s not without risks. Sunburn and skin cancer are still concerns. Sun safety is important for other reasons.
Vitamin D is safe when used right. Sticking to 1,000 to 4,000 IU daily for adults is safe. Rare cases of vitamin d overdose usually come from accidental or intentional overuse.
Following your doctor’s advice and being careful with supplements keeps you safe. This way, you can enjoy vitamin D’s benefits without worry.
Factors That Affect Your Vitamin D Dosage Needs
Not everyone needs the same amount of vitamin D. Several key factors determine your individual requirements. Understanding these factors helps you and your healthcare provider create a supplementation plan that works for you.
Your body’s ability to produce and use vitamin D varies. It depends on biology, lifestyle, and environment. What works for one person might not work for another, even at the same dosage.
Melanin Content and Natural Production
Your skin tone affects how much vitamin D your body produces from sunlight. Melanin, the pigment that gives skin its color, acts as a natural sunscreen. It protects against UV damage but also reduces vitamin D synthesis.[5]
Fair-skinned individuals might produce enough vitamin D from 10-15 minutes of midday sun exposure. But someone with dark brown or black skin might need 30-45 minutes for the same effect. That’s 3 to 5 times longer.
This explains why vitamin D deficiency is more common in people with darker complexions. Research shows that about 70% of African Americans have insufficient vitamin D levels (below 20 ng/mL). Only 30% of Caucasians have the same issue.
The relationship between vitamin d skin tone and production creates a challenge. People with darker skin living in northern climates face a double disadvantage. Both melanin content and low UV exposure work against them.
For optimal natural production, aim for 5-30 minutes of midday sun (10 a.m. to 4 p.m. when UV-B rays are strongest) on exposed skin without sunscreen, at least twice weekly. However, this conflicts with skin cancer prevention advice from dermatologists.
A balanced approach works best for many people. Consider brief vitamin d sun exposure of 10-15 minutes before applying sunscreen, or simply rely on supplementation and consistent sun protection. Sunscreen with SPF 8 or higher blocks vitamin D-producing UV-B rays, though most people don’t apply enough to completely prevent synthesis.
Location and Seasonal Changes
Where you live dramatically impacts your body’s ability to make vitamin D. At latitudes above 37 degrees north—roughly above San Francisco, Denver, and Richmond, Virginia—the sun’s angle from November through February is too low for adequate UV-B to penetrate the atmosphere.
This creates what experts call the “vitamin D winter.” People in Boston, Seattle, Chicago, or anywhere further north get virtually zero vitamin D from sun exposure for 4-6 months each year, regardless of how much time they spend outdoors.
Geographic location affects more than just latitude. Cloud cover, air pollution, and altitude all influence UV-B availability. Mountainous areas receive more UV-B radiation, while polluted urban centers receive less.
| Location Factor | Impact on Vitamin D | Recommendation |
|---|---|---|
| Northern US cities (above 37°N) | Zero synthesis Nov-Feb | Supplement 2000-4000 IU daily in winter |
| Southern US cities (below 37°N) | Year-round synthesis possible | Supplement 1000-2000 IU or regular sun exposure |
| High altitude areas | Increased UV-B exposure | May need less supplementation with sun exposure |
| Polluted urban areas | Reduced UV-B penetration | Rely more on supplementation than sun |
Seasonal variations mean your vitamin D needs change throughout the year. Fall and winter supplementation becomes especially important for northern residents. While year-round supplementation helps people who work indoors or avoid sun exposure.
Body Composition and Storage
The relationship between vitamin d and obesity significantly affects dosage requirements. Vitamin D is fat-soluble, so it gets stored in fat tissue throughout your body. This sounds beneficial, but it actually creates a problem for people carrying extra weight.
In individuals with obesity (BMI over 30), vitamin D becomes sequestered in fat cells. This reduces the amount circulating in your blood where it’s actually needed. Research shows that people with obesity need 2-3 times more vitamin D than normal-weight individuals to achieve the same blood levels.[11]
The Cleveland Clinic developed a predictive equation that beautifully illustrates this relationship. The formula adds 39 IU for each BMI point. Someone with a BMI of 35 needs nearly 1,400 IU more daily than someone with a BMI of 20, based solely on body weight.
Here’s the good news about vitamin d and obesity: absorption doesn’t decrease. Your digestive system processes supplements just fine—you simply need higher doses to compensate for increased fat storage volume.
Body weight considerations include:
- Normal weight (BMI 18.5-24.9): Standard dosage recommendations apply
- Overweight (BMI 25-29.9): Consider 1.5x standard dosage
- Obese (BMI 30-39.9): May need 2-3x standard dosage
- Severely obese (BMI 40+): Often requires 3x or higher dosage
Weight loss can improve vitamin D status through two mechanisms. It releases stored vitamin D back into circulation and reduces the volume of fat tissue sequestering it. Many people see their vitamin D levels improve naturally as they lose weight.
Health Issues and Drug Interactions
Certain medical conditions and medications dramatically alter your vitamin D requirements. These factors often require dosages well above standard recommendations, sometimes under medical supervision.
Malabsorption conditions impair your ability to absorb vitamin D from food and supplements. These include:
- Crohn’s disease and ulcerative colitis
- Celiac disease
- Cystic fibrosis
- Chronic pancreatitis
- Bariatric surgery (gastric bypass, sleeve gastrectomy)
People with these conditions often need much higher doses or even injectable forms of vitamin D. Regular blood testing becomes essential to ensure adequate levels.
Kidney disease creates a unique problem. Your kidneys convert the storage form of vitamin D (25-hydroxyvitamin D) into the active form (calcitriol). When kidneys don’t function properly, this conversion fails. Patients with chronic kidney disease typically need prescription forms of activated vitamin D rather than standard supplements.
Liver disease affects the first step of vitamin D metabolism, where the liver converts dietary vitamin D into 25-hydroxyvitamin D. Severe liver disease may require specialized supplementation strategies.
Several medications interfere with vitamin D metabolism and increase your needs:
- Anticonvulsants (phenytoin, phenobarbital, carbamazepine) speed up vitamin D breakdown
- Glucocorticoids (prednisone, dexamethasone) impair calcium absorption and vitamin D effectiveness
- Some AIDS medications accelerate vitamin D metabolism
- Weight-loss drugs (orlistat/Alli) block fat absorption, including fat-soluble vitamins
- Cholesterol medications (cholestyramine) can reduce vitamin D absorption
If you have any of these conditions or take these medications, discuss vitamin D testing and appropriate supplementation with your doctor. You likely need higher doses than standard recommendations suggest, and regular monitoring ensures you’re getting enough without going overboard.
Understanding your personal risk factors empowers you to work effectively with your healthcare provider. While the RDA provides a helpful baseline, your optimal dose might be quite different based on these individual factors. The key is recognizing what makes your situation unique and adjusting accordingly.
How to Take Vitamin D for Best Absorption
Getting the most out of vitamin D doesn’t need to be hard. Just a few smart steps can make a big difference. Studies show that changing how you take your supplement can boost blood levels by 50% or more.
Understanding how vitamin D works in your body is key. Since it’s a fat-soluble vitamin, it absorbs differently than water-soluble vitamins like vitamin C or B vitamins.[17]
Let’s look at the practical steps that boost vitamin D absorption and effectiveness.
When to Take Your Daily Dose
Timing your supplement right can greatly improve vitamin D absorption. Cleveland Clinic research found that taking vitamin D with the largest meal of the day increased average blood levels by 50.2% compared to taking it on an empty stomach.[16] We have a dedicated deep-dive on the best time to take vitamin D — morning, afternoon, or night — with the full research breakdown.
This is a huge difference from such a simple change! For most Americans, dinner is the biggest meal. So, taking vitamin D in the evening is best. But, if you have a big breakfast or lunch, those work well too. The key is to take vitamin D with food, not on an empty stomach.
Why does meal timing matter so much? Eating activates your digestive system, helping vitamin D absorption. Your gallbladder releases bile acids, your pancreas secretes digestive enzymes, and your intestines form chylomicrons. These tiny fat particles carry vitamin D into your bloodstream.
Daily versus weekly dosing is also important. While weekly high-dose supplements are common, daily dosing might be better for keeping blood levels steady.
The Endocrine Society recommends daily doses of 1,000-4,000 IU with dinner for adults 50 and older. This makes absorption better and keeps your levels consistent.
The Fat Factor for Optimal Absorption
Taking vitamin D with fat is crucial for absorption. The NIH says fat in the gut boosts vitamin D absorption. Vitamin D is mixed with fat particles and about 80% is absorbed through the lymphatic system.
A systematic review found higher blood levels when supplements were taken with meals containing at least 15 grams of fat versus fat-free meals. But what does 15 grams of fat look like in real food?
- A tablespoon of olive oil (14g fat)
- An ounce of nuts like almonds or walnuts (14-18g fat)
- Half an avocado (15g fat)
- A meal with salmon, eggs, or cheese easily provides this amount
- Two tablespoons of peanut butter (16g fat)
You don’t need to measure exactly. Any meal with protein and healthy fats works well. Add nut butter to your toast, have eggs, or include full-fat yogurt at breakfast.
At dinner, any meal with meat, fish, cooking oil, or cheese provides enough fat. Even a glass of whole milk with cereal (8g fat) helps, though low-fat or skim milk won’t do much.
The type of supplement matters less than you think. Whether capsules, softgels, tablets, or liquid drops, all absorb well when taken with food containing some dietary fat.
Nutrient Partnerships That Enhance Results
Vitamin D works with other nutrients for better results. Understanding its partnership with calcium is especially important for bone health.
Vitamin D helps your body absorb calcium from food and supplements. Taking both together is fine. Some experts suggest spacing them out to avoid competition at high doses, but this isn’t necessary for most people.
The relationship between vitamin D and magnesium is increasingly recognized as crucial for optimal health outcomes.
Magnesium is key for converting vitamin D to its active form and for vitamin D to work properly in your cells. Many Americans lack magnesium, which reduces vitamin D’s effectiveness.
Ensure adequate magnesium intake of 320-420 mg daily from food and supplements combined. Good sources include leafy greens, nuts, seeds, whole grains, and legumes.
Vitamin K2 works well with vitamin D and calcium to direct calcium to bones. While not essential, some experts recommend K2 supplementation (90-120 mcg daily) when taking high doses of vitamin D for a long time.
Be cautious with very high doses of vitamin A (above 10,000 IU daily) as it might interfere with vitamin D. Normal multivitamin amounts (3,000-5,000 IU) are fine and won’t cause problems.
Here are practical tips for maximizing your vitamin D supplementation:
- Take your vitamin D daily with your largest meal or any meal with some fat
- Consider a supplement that includes magnesium and K2 for nutrient synergy
- Be consistent with timing to build a sustainable habit
- Don’t stress about perfection—taking it regularly is more important than obsessing over optimal timing
- Track your progress with periodic blood tests to ensure your approach is working
These simple strategies help ensure you get the most from your vitamin D supplementation. Once you establish a routine, these practices become second nature and require no extra effort or thought.
Conclusion
Finding the right vitamin D can be tough with so many guidelines out there. But, the basics are simple. Most adults need 600-800 IU daily for basic health. Many people find they need 1,000-2,000 IU to feel their best.[1]
The 2024 Endocrine Society guidelines say certain groups need more vitamin D. This includes kids and teens, adults over 75, pregnant women, and those with prediabetes. Cleveland Clinic research shows you might need at least 2,000 IU daily to fix a deficiency.[4]
Your needs depend on your age, weight, skin color, where you live, and your health goals. If you’re at risk, like being overweight or having dark skin, getting tested is a good idea. For treating deficiency, taking 5,000 IU daily or 50,000 IU weekly for 8-12 weeks is common. Then, you’ll need to keep up with a smaller dose.[10]
This guide helps you make smart choices about vitamin D supplements. Take your supplement with a meal that has fat for better absorption. The 4,000 IU limit is safe and gives you plenty of room.
Small, steady steps can make a big difference. Whether it’s getting some sun, eating vitamin D-rich foods, or taking supplements, it’s all good. practical guide to vitamin dosages and supplement safety.
Frequently Asked Questions
How much vitamin D should I take daily?▼
The amount of vitamin D you need depends on your age and health. The National Institutes of Health suggests 400 IU for infants and 600 IU for most adults up to 70. Seniors over 70 need 800 IU.
Is 2,000 IU of vitamin D3 too much?▼
No, 2,000 IU of vitamin D3 daily is safe for most adults. The safe upper limit is 4,000 IU daily. Many experts recommend 2,000 IU daily for optimal blood levels.
This dose is more likely to achieve the desired levels than the basic 600 IU RDA. The Cleveland Clinic’s research supports this recommendation.
Can I take 5,000 IU of vitamin D3 every day?▼
Taking 5,000 IU of vitamin D3 daily is safe for many adults. It’s often prescribed for treating deficiency or for those with specific risk factors.
The tolerable upper limit is 4,000 IU daily. However, 5,000 IU is well below the levels that typically cause toxicity. It’s wise to get your blood levels tested before and after starting this dose.
What’s the difference between vitamin D2 and D3, and which should I take?▼
Vitamin D2 comes from plants, while vitamin D3 comes from animals. Vitamin D3 is more potent and effective.
A Cleveland Clinic study found D3 is about 9.5 times more effective. It binds better to proteins, has a longer half-life, and is more efficiently converted to the active form your body needs.
Most healthcare providers recommend D3 supplements over D2. If you’re vegan, look for plant-based D3 derived from lichen.[8]
How do I know if I’m vitamin D deficient?▼
Vitamin D deficiency is diagnosed through a blood test. Levels below 20 ng/mL indicate deficiency. Levels between 20-30 ng/mL suggest insufficiency.
Common symptoms include bone pain, muscle weakness, and mood changes. You’re at higher risk if you have limited sun exposure or darker skin tone.
Discuss testing with your healthcare provider if you suspect deficiency.
Do I need to take vitamin D with food?▼
Yes, taking vitamin D with food improves absorption. Research shows a 50% increase in blood levels when taken with the largest meal of the day.
Vitamin D is fat-soluble, so it absorbs best with dietary fat. Aim for at least 15 grams of fat in your meal for optimal absorption.
For most people, taking vitamin D with dinner works well. Consistency is key—make it a daily habit with a substantial meal.
How long does it take to correct vitamin D deficiency?▼
Correcting vitamin D deficiency takes 8-12 weeks with high-dose supplementation. The standard treatment uses loading doses of 50,000 IU weekly for 8-12 weeks, or 5,000-10,000 IU daily.
After the initial treatment, you’ll need retesting to confirm your levels have reached the sufficient range. Factors like starting level, body weight, and absorption efficiency affect response time.
Once deficiency is corrected, you’ll need ongoing maintenance supplementation. Vitamin D isn’t a one-time fix but an ongoing nutritional need.
Can you get vitamin D toxicity from too much sun exposure?▼
No, you cannot get vitamin D toxicity from sun exposure. Your body has a self-regulating mechanism that prevents toxicity from sunlight.
Vitamin D toxicity almost exclusively results from excessive supplementation. While you can’t get too much vitamin D from sun, you can get too much UV damage.
Should I take vitamin D every day or once a week?▼
For most people, daily dosing is preferred over weekly dosing for long-term supplementation. Daily lower doses may be more effective and safer for long-term use.
The Endocrine Society recommends daily lower doses over non-daily higher doses for adults over 50. Daily dosing provides more consistent blood levels and supports various tissues and systems.
It also reduces the risk of accidentally taking a weekly dose daily, which can lead to toxicity. Taking your vitamin D at the same time each day with a meal builds a sustainable habit.
What vitamin D level should I aim for?▼
There’s ongoing debate about the ideal vitamin D blood level. The official threshold for sufficiency is 20 ng/mL or above.
However, many experts recommend targeting 30-50 ng/mL for optimal health benefits. The Cleveland Clinic suggests maintaining levels of 40-60 ng/mL for immune system support.
Levels between 20-30 ng/mL are considered “insufficient” by some experts. Most agree that levels above 50 ng/mL offer no additional proven benefits.
A practical target for most people is 30-40 ng/mL—high enough to support bone health and immune function, while remaining safely below concerning levels.
Do breastfed babies need vitamin D supplements?▼
Yes, exclusively and partially breastfed babies need vitamin D supplementation starting in the first days of life. Breast milk contains very little vitamin D.
The American Academy of Pediatrics recommends 400 IU daily for all breastfed infants. Formula-fed babies typically don’t need supplements because formula is fortified with vitamin D.
Supplementation is safe and effectively prevents rickets, a serious bone disease. It’s essential to ensure adequate vitamin D levels in breastfed babies.
Does body weight affect how much vitamin D I need?▼
Yes, body weight significantly affects vitamin D requirements. Vitamin D is fat-soluble and gets stored in fat tissue, reducing the amount in the bloodstream.
Research shows that individuals with obesity need 2-3 times more vitamin D than normal-weight people. The Cleveland Clinic’s predictive equation illustrates this clearly.
It’s best to consider higher doses of 2,000-4,000 IU daily for those with a BMI over 30. Discuss testing with your healthcare provider to ensure you’re reaching adequate blood levels.
Can vitamin D help with depression and mood?▼
Vitamin D may help with depression and mood disorders, though the research shows mixed results. There’s a biological rationale for this.
Vitamin D receptors exist in brain areas that regulate mood and behavior. Deficiency has been linked to seasonal affective disorder (SAD), depression, and other mood disturbances.
Some studies show that vitamin D supplementation improves depressive symptoms, particularly in people with documented deficiency or seasonal depression. However, other intervention trials haven’t found consistent benefits.
The connection appears strongest for SAD, where reduced sunlight exposure in winter months contributes to both low vitamin D and mood changes. If you experience winter blues, depression, or mood issues, it’s worth discussing vitamin D testing with your healthcare provider.
What are the symptoms of vitamin D toxicity?▼
Vitamin D toxicity symptoms result from hypercalcemia (too much calcium in the blood) rather than from vitamin D itself. Early symptoms include nausea, vomiting, weakness, frequent urination, and excessive thirst.
Moderate symptoms involve bone pain, kidney problems (including stones), digestive issues like constipation or stomach pain, and heart rhythm abnormalities. Severe toxicity can cause confusion, disorientation, kidney failure, and serious heart problems.
A Cleveland Clinic case study illustrates this: an 80-year-old man who accidentally took 50,000 IU daily instead of weekly developed calcium levels of 14.4 mg/dL and vitamin D levels of 365 ng/mL, experiencing nausea, weakness, and confusion. His condition resolved completely after stopping the supplement and receiving treatment for high calcium.
How does skin tone affect vitamin D production?▼
Skin tone dramatically affects how efficiently your body produces vitamin D from sunlight. Melanin, the pigment that gives skin its color, acts as a natural sunscreen that protects against UV damage but also reduces vitamin D synthesis.
People with darker skin need 3-5 times longer sun exposure to produce the same amount of vitamin D as fair-skinned individuals. While someone with fair skin might generate adequate vitamin D from 10-15 minutes of midday sun exposure, a person with dark brown or black skin might need 30-45 minutes for equivalent production.
This biological difference helps explain why vitamin D deficiency is much more common in people with darker complexions. If you have darker skin, especially if you live in northern latitudes or spend most time indoors, you’re at higher risk for deficiency and likely benefit from year-round supplementation with at least 1,000-2,000 IU daily, possibly more.
Should I take vitamin D with calcium?▼
Vitamin D and calcium work synergistically. Vitamin D helps your body absorb calcium from food and supplements, while calcium is essential for the bone-building processes that vitamin D supports.
For bone health and osteoporosis prevention, you need adequate amounts of both. Typically, 1,000-1,200 mg of calcium daily plus 800-2,000 IU of vitamin D is recommended. You can take them together without problems, as they complement each other.
Some experts suggest spacing them out (calcium with one meal, vitamin D with another) at very high doses to avoid potential absorption competition. However, this is probably unnecessary at typical supplementation levels. More important than timing is ensuring you’re getting enough of both.
Many older adults, especially post-menopausal women, benefit from combination supplements that provide both nutrients in appropriate ratios. If you’re taking both separately, consider calcium with breakfast and vitamin D with your largest meal (often dinner) to optimize vitamin D absorption with dietary fat.
Can I get enough vitamin D from food alone?▼
Getting enough vitamin D from food alone is challenging for most people. Very few foods naturally contain significant amounts of vitamin D.
The richest natural sources are fatty fish like salmon, mackerel, and sardines, plus egg yolks. In the United States, fortified foods provide most dietary vitamin D: fortified milk, fortified plant milks, fortified breakfast cereals, and fortified orange juice.
Even eating these foods regularly typically provides only 200-400 IU daily—well below the 600 IU RDA for most adults. To get 600 IU from food alone, you’d need to drink 5 cups of fortified milk daily or eat salmon almost every day, which isn’t practical or affordable for most people.
This is why supplementation has become so important—it’s the most reliable way to ensure adequate vitamin D intake, especially for people with limited sun exposure. If you prefer getting nutrients from food, focus on fatty fish several times weekly, fortified dairy or plant milks, and eggs, but consider a modest supplement (1,000-2,000 IU) to fill the gap.
Does vitamin D help prevent colds and flu?▼
Research suggests that adequate vitamin D levels may help reduce the risk of respiratory infections, including colds and flu, though it’s not a guaranteed prevention. Vitamin D receptors are present throughout the immune system, and vitamin D plays important roles in activating immune defenses against infections.
Cleveland Clinic reviews show that vitamin D helps regulate both innate immunity (your body’s immediate response to pathogens) and adaptive immunity (longer-term, targeted responses). Multiple studies have found that people with low vitamin D levels experience more frequent respiratory infections, and some intervention trials show that vitamin D supplementation reduces the incidence of colds, flu, and other respiratory illnesses, particularly in people who were deficient to begin with.
The effect appears strongest in individuals with baseline levels below 20 ng/mL. While vitamin D supplementation won’t eliminate your risk of getting sick, maintaining adequate levels (at least 30 ng/mL, possibly 40-60 ng/mL for immune optimization) through supplementation of 1,000-4,000 IU daily may provide some protective benefit, especially during cold and flu season. Consider it one component of a comprehensive immune support strategy that also includes good nutrition, adequate sleep, stress management, hand washing, and vaccination where appropriate.
What’s the best time of day to take vitamin D?▼
The best time to take vitamin D is with your largest meal of the day, which for most Americans is dinner. Cleveland Clinic research demonstrated that taking vitamin D with the largest meal increased blood levels by 50% compared to taking it on an empty stomach—a significant difference from such a simple timing change.
Vitamin D is fat-soluble, so it absorbs best when taken with food, particularly meals containing at least 15 grams of fat. Your largest meal typically provides the most dietary fat, optimizing absorption. Additionally, taking supplements at the same time each day builds a consistent habit, making it easier to remember.
If breakfast or lunch is your largest meal, that’s perfectly fine—the key is pairing it with substantial food and fat rather than taking it on an empty stomach. Some people prefer morning supplementation because taking fat-soluble vitamins later in the day might theoretically affect sleep (though there’s limited evidence for this with vitamin D), while others find evening dosing easier to remember as part of their dinner routine. Choose whichever meal timing works best for your lifestyle and stick with it consistently. The most important factors are building a consistent daily supplement routine and making it a sustainable habit.
Do I need to take magnesium with vitamin D?▼
While not absolutely required, taking adequate magnesium when supplementing with vitamin D is increasingly recognized as important for optimal vitamin D function. Magnesium is necessary for converting vitamin D to its active form and for vitamin D to work properly in your cells—it’s involved in virtually every step of vitamin D metabolism.
Research suggests that many Americans are magnesium-deficient (getting less than the recommended 320-420 mg daily), and this deficiency may limit how effectively your body can use vitamin D, potentially explaining why some people don’t respond well to supplementation. Some studies show that adequate magnesium status improves vitamin D levels and that magnesium deficiency can actually impair vitamin D metabolism.
For these reasons, magnesium supplementation for sleep and muscle recovery—either through magnesium-rich foods like nuts, seeds, whole grains, leafy greens, and legumes, or through supplementation (200-400 mg daily)—makes sense when taking vitamin D, especially at higher doses. Many combination supplements now include both nutrients. Additionally, vitamin K2 and its synergy with vitamin D for bone health to work synergistically with vitamin D in directing calcium to bones rather than soft tissues, though this is less critical than magnesium. Consider magnesium an important supporting nutrient that helps you get maximum benefit from your vitamin D supplementation.[12]
Related Reading
Sources
- NIH Office of Dietary Supplements — Vitamin D Fact Sheet
- National Academies of Sciences — Dietary Reference Intakes for Calcium and Vitamin D
- Remedy’s Nutrition — How Vitamin D Needs Change Through Different Life Stages
- Endocrine Society — Vitamin D for Prevention of Disease (2024 Guidelines)
- PubMed — Vitamin D Deficiency Prevalence in US Adults
- PubMed — Vitamin D Supplementation in Elderly Patients
- PubMed — Vitamin D Requirements During Pregnancy
- PubMed — Vitamin D3 vs D2: Comparative Effectiveness
- PubMed — Vitamin D and Bone Health: A Review
- PubMed — Vitamin D Toxicity and Hypercalcemia
- PubMed — Body Weight and Vitamin D Requirements
- PubMed — Magnesium and Vitamin D Metabolism
- PubMed — Vitamin D and Immune Function
- Mayo Clinic — Vitamin D: Dosage and Safety
- Harvard Health Publishing — Vitamin D and Your Health
- Cleveland Clinic — Vitamin D Deficiency: Symptoms and Causes
- Healthline — How Much Vitamin D Should You Take?
- WebMD — Vitamin D Deficiency: Symptoms, Causes and Treatment
- Medical News Today — Vitamin D: Health Benefits, Facts and Research
- Linus Pauling Institute — Vitamin D Overview
- American Academy of Pediatrics — Vitamin D for Infants and Children
