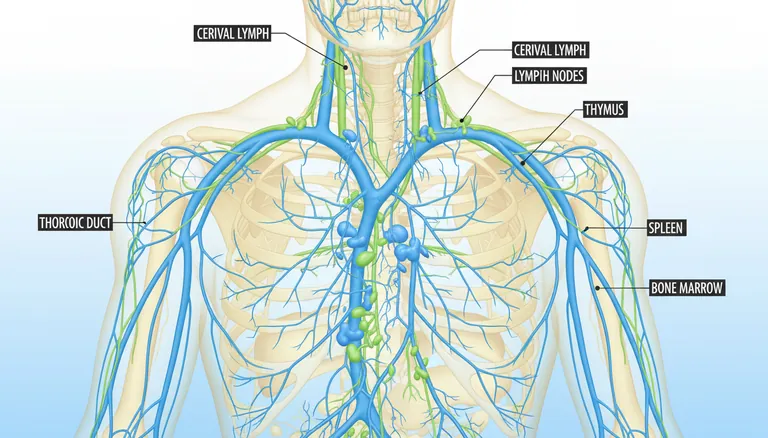
Your body has a hidden network working beneath your skin that rarely gets the attention it deserves. This network, called the lymphatic system, acts like your body’s personal cleanup crew. It filters out waste, bacteria, and other unwanted materials that can make you feel sluggish or unwell.
Think of it as a sophisticated drainage system running throughout your entire body. Tiny tubes called vessels collect fluid and carry it through checkpoints known as lymph nodes. These nodes house immune cells that destroy harmful substances before they can cause problems.
Lately, you’ve probably heard about lymphatic drainage becoming popular in wellness circles. While it might seem like just another health trend, there’s real science behind supporting your lymph health. Whether you’re dealing with swelling, want to boost immune support, or simply feel curious about optimizing your body’s natural systems, understanding how this works matters.
This guide will walk you through everything you need to know about manual lymphatic drainage, its proven benefits, and practical ways to keep your system running smoothly.
Quick Answer: What Is Lymphatic Drainage?
Lymphatic drainage refers to the natural circulation of lymph fluid through your body’s lymphatic system — and to the therapeutic techniques designed to support that flow. Manual lymphatic drainage (MLD) is a clinically validated, gentle massage technique used to reduce swelling, support post-surgical recovery, and strengthen immune function. At home, you can support lymphatic health through movement, hydration, anti-inflammatory nutrition, breathwork, and tools like dry brushing. For those with lymphedema or chronic swelling, professional MLD performed by a certified lymphedema therapist is the gold standard of care.
Key Takeaways
- Your lymphatic system removes waste and supports immune function by filtering harmful substances through lymph nodes
- Manual lymphatic drainage uses gentle techniques to encourage fluid movement and reduce swelling
- Supporting lymph health can help with immune support, post-surgery recovery, and overall wellness
- The system relies on movement and muscle contractions since it lacks a pump like the heart
- Both professional treatments and at-home practices can benefit your lymphatic circulation
- Understanding proper techniques ensures safe and effective results
Understanding Your Lymphatic System and Why It Matters
Underneath your skin, a vast network works tirelessly. It’s crucial for your health but often overlooked. Learning about your lymphatic system can help you take better care of yourself.[1]
Your lymphatic system fights infections and removes waste. It’s as important as your heart and lungs.
The Body’s Hidden Highway
The lymphatic system is a network of vessels and organs. It’s like your body’s sanitation and defense team. It quietly collects waste and harmful substances.[2]
It’s connected to your immune response. The system houses immune cells that fight off threats. These cells are like security guards in your body.
The lymphatic system is vital but often overlooked. It’s absolutely essential for your health.
Building Blocks of Your Lymphatic Network
Your lymphatic system has three main parts. Each part has a specific role. Understanding these parts helps you see how the system works.
Lymph nodes are small organs in your body. They filter lymph fluid for harmful substances. Immune cells inspect the fluid in these nodes.
Lymphatic vessels are tiny tubes that transport lymph fluid. They start small and get bigger, like streams merging into rivers. This network is extensive, running parallel to your blood vessels.
Lymph fluid is a clear liquid that bathes your tissues. It picks up waste and carries it for elimination. It contains white blood cells and proteins.
| Component | Primary Function | Key Locations | What It Contains |
|---|---|---|---|
| Lymph Nodes | Filter and trap harmful substances | Neck, armpits, groin, abdomen | Immune cells, lymphocytes, macrophages |
| Lymphatic Vessels | Transport lymph fluid throughout body | Parallel to blood vessels in all tissues | Smooth muscle walls, one-way valves |
| Lymph Fluid | Collect waste and deliver immune cells | Tissue spaces and vessel channels | White blood cells, proteins, cellular waste |
| Lymphoid Organs | Produce and mature immune cells | Spleen, thymus, tonsils, bone marrow | Developing lymphocytes, antibodies |
The vessels collect fluid, the lymph nodes filter it, and the lymph fluid carries everything back to your bloodstream. Your kidneys then process it.
Two Systems, Different Jobs
Many confuse the lymphatic system with the circulatory system. But they have distinct purposes and mechanisms.
The circulatory system relies on your heart to pump blood. Your heart beats about 100,000 times daily. It delivers oxygen and nutrients and removes carbon dioxide.
The lymphatic system has no central pump. It depends on muscle contractions and breathing to flow. When you move, your muscles push lymph fluid forward through one-way valves.
The lymphatic system is really part of the immune system—it’s part of how your body recognizes and attacks abnormal cells with mutations.
The circulatory system is a closed loop. Blood continuously circulates from the heart. The lymphatic system is a one-way drainage system. It collects excess fluid and returns it to the bloodstream near your heart.
Blood carries oxygen-rich red blood cells. Lymph fluid contains white blood cells for immune defense. The circulatory system focuses on nutrient delivery, while the lymphatic system focuses on waste removal and immune surveillance.
Exercise is key for lymphatic health. Without a heart pump, your lymph fluid relies on your activity to flow. This makes lifestyle choices crucial for your lymphatic health.
The Essential Role of Lymphatic Drainage in Your Body
Your lymphatic system works quietly behind the scenes. It does important tasks, even when you’re sleeping. When it works well, you might not even notice. But if it doesn’t, you’ll definitely feel it.
Understanding your lymphatic system is key to why it’s so important. It plays two main roles in keeping you healthy and feeling good.
Your Body’s Sanitation Department
Your lymphatic system is like a garbage disposal service for your body. Every day, your cells make waste as they work. This waste includes damaged cells, bacteria, viruses, and toxins.[3]
Waste removal is a constant process in your body. Your lymph vessels collect waste and take it to lymph nodes. These nodes filter out harmful substances.
People often talk about detoxification in terms of cleanses or diets. But your body has a real detox system. The lymphatic system removes unwanted materials from your tissues.
This system deals with:
- Bacteria and viruses that enter your body or multiply within it
- Dead or damaged cells that need to be cleared away
- Abnormal cells that could potentially become cancerous
- Metabolic waste products from normal cellular activities
- Toxins from environmental exposure or food
All cells need lymph fluid to boost immunity and remove waste. Without it, harmful materials build up, causing inflammation, infection, and disease.
Maintaining the Right Amount of Fluid
Your lymphatic system also helps keep your body’s fluid balance right. This might seem simple, but it’s crucial for your health and comfort.
Fluid balance works like this: Fluid leaks from your capillaries into tissues. This fluid, called interstitial fluid, delivers nutrients to your cells. But not all of it goes back to your blood vessels.
Your lymphatic vessels collect the extra fluid. They turn it into lymph and return it to your bloodstream near your heart. This keeps your tissues from getting too wet.[6]
When your lymphatic system works well, you stay balanced. You don’t get swollen, and your tissues get the nutrients they need. The system processes about 2-4 liters of fluid every day, keeping it in a continuous cycle.
Fluid balance problems show up fast. If your lymphatic system fails, fluid builds up in your tissues. This causes swelling, especially in your arms, legs, or face. The swelling can be mild or severe, affecting how you move and feel.
The link between lymph circulation and health goes beyond preventing swelling. Proper fluid balance ensures your cells get nutrients, waste doesn’t build up, blood volume stays stable, and your immune system works well.
Your lymphatic system works with your circulatory system. Together, they keep your body’s internal environment stable and healthy. This supports every other system in your body.
Lymphatic Drainage Benefits for Overall Health
Supporting your lymphatic system offers many health benefits that are often overlooked. It strengthens your body’s defenses and helps you recover faster after surgery. When your lymphatic system works well, you’ll feel better, heal faster, and look healthier.
Your lymphatic system is key to staying healthy. It carries white blood cells that fight diseases. Let’s look at how it supports your health goals. Research also highlights how vitamin D and immune system health are closely intertwined with lymphatic activity.
Boosting Immune System Function
Your lymphatic system is a primary defense against illness. Lymph nodes are like command centers where immune cells gather. They help fight off threats by moving quickly to where they’re needed.[4]
Lymph nodes act like checkpoints, filtering out harmful substances. When lymphatic flow improves, your immune system gets a boost. This lets your body’s defenders work better.[5]
Studies show lymphatic drainage massage can increase lymphocytes. These cells are crucial in fighting infections and keeping your body safe.
Reducing Inflammation and Swelling
One big benefit is reducing swelling and inflammation. When tissues get inflamed, fluid builds up. Your lymphatic vessels help remove this fluid, taking inflammatory substances with it.
For those with lymphedema or chronic inflammation, improving lymphatic flow is very important. Manual lymphatic drainage can remove trapped fluid, reducing swelling in arms, legs, and more.
This effect goes beyond visible swelling. Proper lymphatic function helps tissues heal faster and reduces pain from chronic inflammation.
Improving Skin Health and Appearance
Your skin benefits a lot when lymphatic circulation is good. It reduces puffiness around your eyes and jawline. This makes you look more defined and refreshed.
Many people see clearer, healthier skin after trying lymphatic drainage. It removes toxins and waste, helping prevent breakouts and improve skin tone. Better circulation also means more nutrients for your skin.
Professional aestheticians often use lymphatic massage in facial treatments. It helps:
- Decrease under-eye bags and facial puffiness
- Promote a natural, healthy glow
- Support the skin’s natural detoxification processes
- Reduce the appearance of fine lines caused by fluid retention
Supporting Post-Surgical Recovery
Lymphatic drainage is essential for recovery after surgery. Surgery can disrupt lymphatic pathways, causing swelling and slower healing. Gentle massage helps restore fluid flow and speeds up healing.
Studies suggest lymphatic drainage improves recovery after surgery. It’s especially helpful for cosmetic procedures like liposuction, breast augmentation, and facelifts. Patients often experience less swelling and faster recovery times.
The benefits of lymphatic drainage extend beyond cosmetic procedures. It helps those recovering from orthopedic surgeries, cancer treatments, or other medical interventions. It reduces fluid buildup after tissue trauma.
Healthcare providers are increasingly recognizing the value of lymphatic support in recovery plans. Always talk to your surgeon or healthcare provider before starting lymphatic drainage therapy after surgery.
Signs Your Lymphatic System May Need Support
Your body often sends clear signals when your lymphatic system needs extra attention and care. Learning to recognize these lymphatic system symptoms can help you take early action and prevent more serious complications down the road. While occasional puffiness or temporary swelling can be normal, persistent symptoms may indicate that your lymph system requires additional support.
The good news is that many signs of poor lymphatic function are reversible with the right interventions. By paying attention to what your body is telling you, you can address issues before they become more challenging to manage.
What Your Body Tells You About Lymphatic Health
The most obvious sign that your lymphatic system isn’t working optimally is swelling in your arms or legs. This condition, known as lymphedema, happens when fluid that should be drained by your lymph vessels builds up instead. You might notice that your rings suddenly feel tight on your fingers, or your favorite shoes no longer fit comfortably by the end of the day.[2]
These lymphedema symptoms often start subtly. Your clothes may feel a bit snugger around your arms, legs, or waist. You might experience a sensation of heaviness or tightness in your limbs, even when you haven’t been particularly active.[12]
Beyond swelling, your body may signal lymphatic dysfunction through other noticeable changes. Frequent infections, especially in the same area repeatedly, can indicate that your immune system isn’t getting the support it needs from proper lymph flow. Wounds that heal more slowly than expected might also point to compromised lymphatic function.
Many people with poor lymphatic function experience persistent fatigue that doesn’t improve with rest. Morning stiffness that takes longer than usual to resolve can be another clue. You might also notice skin changes, such as a feeling of tightness, texture changes, or a shiny appearance in affected areas.
Other common symptoms include:
- Unexplained aches and discomfort in your limbs
- A general feeling of puffiness or bloating
- Reduced flexibility or range of motion
- Skin that feels harder or thicker than normal
- Recurring infections in the same area
- Brain fog or difficulty concentrating
As lymphatic congestion becomes more advanced, you may have trouble wearing jewelry comfortably. Bracelets, rings, and watches that once fit perfectly might leave indentations in your skin. In more serious cases, you could develop infections in the affected limb that require medical attention.
Who’s at Greater Risk for Lymphatic Problems
Certain factors can increase your likelihood of experiencing lymphatic system symptoms and dysfunction. Understanding these risk factors helps you stay vigilant and take preventive measures when possible.
Cancer treatment represents one of the most significant risk factors for lymphatic problems. If you’ve had lymph nodes removed during surgery or received radiation therapy near lymph node areas, your risk of developing lymphedema increases substantially. The lymphatic system can be permanently altered by these treatments, making drainage less efficient.
Surgery of any kind, particularly in areas with concentrated lymph nodes like the groin, armpit, or neck, can disrupt normal lymph flow. Injury or trauma to lymphatic vessels from accidents or repetitive motion can also compromise function over time.
| Risk Factor Category | Specific Conditions | Impact Level |
|---|---|---|
| Cancer-Related | Lymph node removal, radiation therapy, chemotherapy | High |
| Lifestyle Factors | Obesity, prolonged sitting, lack of physical activity | Moderate to High |
| Medical Conditions | Chronic venous insufficiency, infections, rheumatoid arthritis | Moderate |
| Genetic/Inherited | Primary lymphedema, Milroy’s disease, lipedema | Variable |
Obesity significantly affects lymphatic function because excess weight puts additional pressure on lymph vessels and can slow drainage. Similarly, prolonged periods of immobility—whether from bed rest, sitting at a desk all day, or limited mobility—reduce the natural pumping action that keeps lymph flowing.
Chronic venous insufficiency, where veins struggle to send blood back to your heart, often goes hand-in-hand with lymphatic dysfunction. The two systems work together, so when one struggles, the other often does too.
Certain chronic conditions can also contribute to poor lymphatic function. People with rheumatoid arthritis, fibromyalgia, or chronic fatigue syndrome may experience lymphatic congestion as part of their overall condition. Lipedema, a condition involving abnormal fat distribution, can also impair lymph drainage.
Rare inherited conditions like primary lymphedema or Milroy’s disease affect the lymphatic system from birth or early childhood. While less common, these conditions require specialized medical management and ongoing support.
Recurrent infections, particularly cellulitis or lymphangitis, can damage lymphatic vessels over time and create a cycle where poor drainage leads to more infections. Breaking this cycle requires attention to both treating infections promptly and supporting overall lymphatic health.
The encouraging news is that even with risk factors present, many people can maintain good lymphatic function through lifestyle choices and early intervention. Recognizing symptoms early and taking appropriate action often leads to better outcomes and helps prevent progression to more serious stages of lymphatic dysfunction.
What Is Manual Lymphatic Drainage Therapy?
Manual lymphatic drainage is different from other massage therapies. It uses extremely gentle touch and precise movements to help your lymph fluid flow better. This therapy focuses on the lymphatic vessels under your skin, not the muscles.
MLD therapy is a recognized medical treatment used by certified therapists worldwide. The technique involves light, rhythmic strokes that gently stretch the skin in the direction of lymph flow. This creates a pumping effect that helps move fluid through your system.[19]
Origins and Evolution of This Specialized Technique
The story of manual lymphatic drainage starts in the 1930s with Danish physician Dr. Emil Vodder and his wife Estrid. They noticed that people with chronic colds and sinus infections had swollen lymph nodes in their necks.[13]
Touching lymph nodes was seen as medically inappropriate back then. But the Vodders thought gentle massage might help these swollen nodes drain more effectively.
They started experimenting with light, circular movements and saw remarkable improvements in their patients. Over the years, they refined their approach and developed the Vodder technique. By the 1960s, manual lymphatic drainage was recognized in Europe as a legitimate therapy.
In the 1970s, German physician Dr. Michael Földi advanced the field by incorporating MLD therapy into a comprehensive treatment program for lymphedema. His work helped establish lymphatic massage therapy as a key part of modern lymphedema management. Complementary approaches such as modified citrus pectin for immune and detox support have since gained attention for their role in lymphatic wellness.
The Science Behind Professional Treatment
Professional manual lymphatic drainage works through a carefully orchestrated sequence of movements. It might seem counterintuitive at first. Instead of starting where you have swelling, trained therapists begin by clearing the central lymph node areas in your neck, armpits, and groin.
This approach creates space in your lymphatic system where congested fluid can flow. It’s like unclogging a drain from the bottom up rather than pushing more water down from the top.
The pressure used during MLD therapy is remarkably light—typically less than 9 ounces of pressure, which is about the weight of a nickel. This gentle touch stimulates the lymphatic vessels without compressing them or affecting the deeper muscle tissue. Therapists use their hands to create a wave-like motion that encourages lymph fluid to move toward functioning lymph nodes.
Each stroke follows the natural direction of lymph flow in your body. The therapist systematically works through different body regions, always moving fluid toward areas where your lymphatic system can process and eliminate it effectively.
Comparing the Vodder and Földi Approaches
Today, two primary methods dominate professional practice: the Vodder technique and the Foldi method. While both approaches share the same fundamental goal, they differ in their specific movements and treatment sequences.
The Vodder technique uses four basic strokes: stationary circles, pump technique, rotary technique, and scoop technique. These movements create a gentle pumping action that stimulates lymphatic vessels. Practitioners perform circular motions with varying hand positions depending on the body area being treated.
The Foldi method incorporates similar principles but follows a more structured protocol. This approach combines circular movements with a specific sequential pattern that Dr. Földi developed through clinical research. It often integrates compression bandaging and exercise as part of a comprehensive treatment plan.
| Aspect | Vodder Technique | Földi Method |
|---|---|---|
| Primary Movements | Four basic strokes: stationary circles, pump, rotary, and scoop techniques | Circular movements with structured sequential protocols |
| Treatment Approach | Focuses on rhythmic, pumping motions adapted to specific body areas | Systematic sequence combined with comprehensive lymphedema therapy |
| Pressure Application | Very light touch with gentle skin stretching | Light pressure following specific directional patterns |
| Best Suited For | General lymphatic support, post-surgical care, wellness treatments | Complex lymphedema cases, medical conditions requiring structured protocols |
| Additional Components | Primarily manual techniques | Often includes compression therapy and exercise prescriptions |
Both techniques require specialized training and certification. Therapists typically complete 135-160 hours of coursework to become qualified in lymphatic massage therapy. This extensive education ensures they understand the anatomy of your lymphatic system, recognize contraindications, and can adapt treatments to individual needs.
The choice between techniques often depends on your specific condition and your therapist’s training. Some practitioners combine elements from both approaches to create a customized treatment plan. What matters most is that your therapist has proper certification and experience working with the lymphatic system.
Understanding these foundational techniques helps you appreciate that manual lymphatic drainage is far more than a relaxing spa treatment. It’s a scientifically-based therapeutic intervention that requires skill, knowledge, and precision to perform effectively.
Professional Lymphatic Drainage Massage: What to Expect
Professional lymphatic drainage massage offers specialized care that goes beyond what you can achieve on your own. Understanding the process helps you make the most of this therapeutic treatment. Working with a trained expert ensures you receive safe, effective care tailored to your specific needs.
Whether you’re managing lymphedema, recovering from surgery, or simply looking to support your body’s natural detoxification, knowing what to expect can make your experience more comfortable and rewarding.[18]
The journey to better lymphatic health often starts with finding the right professional. Once you connect with a qualified therapist, you’ll discover a personalized approach that addresses your unique concerns and goals.
Finding a Qualified Lymphatic Drainage Therapist
Choosing the right lymphatic drainage therapist is essential for getting safe and effective treatment. Look for professionals who have completed specialized training in manual lymphatic drainage techniques. A certified lymphedema therapist (CLT) represents the gold standard, especially if you’re dealing with lymphedema or post-surgical swelling.
These specialists complete extensive coursework and hands-on training in lymphatic system anatomy and therapeutic techniques. Many physical therapists and massage therapists also pursue MLD certification to offer this specialized service.
When searching for a qualified professional, ask about their credentials and training background. Inquire whether they’ve studied recognized methods like the Vodder or Földi techniques. Experience matters, so don’t hesitate to ask how long they’ve been practicing and whether they have experience with your specific condition.

Your healthcare provider can be an excellent resource for referrals to trusted practitioners. You can also search professional directories through organizations like the Lymphology Association of North America (LANA) or the National Lymphedema Network. These organizations maintain databases of certified professionals in your area.
Consider scheduling a brief consultation before committing to treatment. This gives you a chance to ask questions, discuss your goals, and ensure you feel comfortable with the therapist’s approach and personality.
Your First Session: The Process
Your first MLD session typically begins with a thorough consultation and health history review. The lymphatic drainage therapist will ask about your medical background, current symptoms, medications, and treatment goals. This information helps them create a personalized treatment plan that addresses your specific needs.
Before beginning the actual massage, your therapist will perform a detailed assessment. They’ll examine areas of swelling, evaluate your skin condition, and check for any contraindications that might affect treatment. This initial evaluation ensures your safety and helps establish a baseline for measuring progress.
The professional lymphatic massage itself feels quite different from traditional massage. You’ll remain fully or partially clothed, depending on the treatment area. The therapist uses gentle, rhythmic movements with very light pressure to encourage lymph flow.
Most MLD sessions last between 45 and 60 minutes. The therapist typically starts at the neck and chest area to clear the central lymphatic pathways before moving to other body regions. The strokes follow specific patterns that direct lymph fluid toward functioning lymph nodes.
Many people find the experience deeply relaxing, though some feel unusual sensations as fluid begins moving. You might notice gurgling sounds in your abdomen or feel slightly lightheaded. These reactions are normal and indicate the treatment is working.
After your session, your therapist may teach you self-massage techniques to practice at home. They might also provide guidance on compression garments, exercise, or other supportive measures. Drinking plenty of water after treatment helps support the drainage process.
How Often Should You Get Professional Treatment?
Treatment frequency varies significantly based on your individual condition and goals. There’s no one-size-fits-all answer, and your certified lymphedema therapist will develop a personalized schedule based on your specific situation.
For people managing chronic lymphedema, intensive treatment might involve multiple sessions per week during the initial phase. This approach helps reduce swelling and establish better lymphatic flow. Once swelling decreases, maintenance sessions might drop to once or twice monthly.
Post-surgical recovery typically requires a shorter treatment course. Someone recovering from cosmetic surgery or lymph node removal might benefit from 3 to 6 sessions over several weeks. The exact treatment frequency depends on healing progress and swelling patterns.[15]
Those using professional lymphatic massage for general wellness or minor swelling might find monthly sessions sufficient. Some people schedule quarterly appointments as preventive care, while others seek treatment only when symptoms appear.
| Condition | Initial Phase Frequency | Maintenance Phase | Typical Duration |
|---|---|---|---|
| Chronic Lymphedema | 3-5 times per week | 1-2 times per month | Ongoing management |
| Post-Surgical Recovery | 2-3 times per week | As needed | 3-8 weeks |
| General Wellness | 1-2 times per month | Monthly or quarterly | Ongoing support |
| Acute Inflammation | 2-4 times per week | Weekly then monthly | 4-12 weeks |
Your therapist will monitor your response to treatment and adjust the schedule accordingly. Some people progress quickly and need fewer sessions than expected. Others require more intensive or prolonged care to achieve their goals.
Insurance coverage may also influence treatment frequency. Many insurance plans cover MLD sessions when prescribed by a physician for medical conditions like lymphedema. Check with your insurance provider to understand your benefits and any session limits.
Remember that professional treatment works best when combined with self-care practices. Your therapist will likely encourage you to practice self-massage techniques, wear compression garments if appropriate, stay active, and maintain good hydration between sessions. This comprehensive approach maximizes the benefits of professional lymphatic massage and supports long-term lymphatic health.
Self-Lymphatic Drainage Techniques You Can Do at Home
Self-lymphatic drainage is a simple way to keep your lymphatic system flowing. It helps with swelling, boosts your immune system, and improves overall health. But, it’s key to learn the right techniques to avoid harming your lymphatic system.[14]
Lymphatic self-massage is easy and accessible. You don’t need fancy tools or a lot of time. Just a few minutes each day can make a big difference in how you feel.
Preparing for Self-Massage
Before starting your home lymphatic drainage, proper preparation is crucial. First, learn the correct technique from a qualified professional. A therapist trained in manual lymphatic drainage can teach you safely.
After learning, create a comfortable setting. Sit or lie down in a relaxed position. Make sure your skin is clean and dry, as lymphatic massage works on the skin’s surface.
Never use oils, lotions, or creams during your session. These products can hinder the gentle skin-stretching needed for effective drainage. Moisturize after your routine.
Understanding pressure is key. Use only enough pressure to gently move the skin without pressing too hard. Aim for the weight of a nickel on your skin.
Neck and Chest Drainage Techniques
Your neck and chest are key areas for lymphatic drainage. They’re great starting points for any self-lymphatic drainage session. These techniques activate the lymph capillaries and prepare your system to receive fluid.
Start by tapping the area above your collarbones with light pressure. Use your fingertips for soft, rhythmic taps for 10-15 seconds on each side. This activates the lymph capillaries and signals your lymphatic system to move.
Next, place your hands flat on the sides of your neck. Use gentle pressure to stroke downward toward your collarbones in a slow motion. Repeat this 5-10 times, always moving toward your heart.
For the chest, create C-shaped movements with your fingers. Start near your armpits and sweep across your chest toward the center. These circular motions should be soft and rhythmic, never rushed or forceful.
Arms and Legs Drainage Methods
When working on your limbs, always follow the golden rule: work from the extremities toward your trunk. This ensures lymph fluid moves toward major drainage points rather than away.
For your arms, start by clearing the lymph nodes in your armpits. Place your hand in your armpit and gently pump with light pressure 5-10 times. Then, begin at your wrist and use gentle, sweeping strokes moving up toward your elbow, then from your elbow to your shoulder.
The movements should create a gentle C-shape or wave pattern as you guide your hand along your arm. Take your time with each stroke, counting slowly to three as you complete each sweep. Repeat this sequence 3-5 times on each arm.
Leg drainage follows the same principle. Begin by activating the lymph nodes in your groin area with gentle circular movements. Then start at your ankle and work upward in sections—ankle to knee, then knee to thigh—using those same light, sweeping C-shaped motions.
Remember that gravity makes leg drainage particularly important. If you spend long hours sitting or standing, these DIY lymphatic massage techniques can help prevent fluid buildup and reduce that heavy, tired feeling in your legs.
Abdominal Lymphatic Massage
Your abdomen contains a significant portion of your lymphatic system, making abdominal massage a valuable addition to your self-care routine. This area responds particularly well to gentle, circular movements that follow your body’s natural digestive pathway.
Lie on your back in a comfortable position with your knees slightly bent. Place both hands flat on your lower right abdomen, just above your hip bone. Using light pressure, move your hands in a clockwise circular motion—this direction follows the path of your intestines and encourages proper lymphatic flow.
Start with small circles in the lower right area, then gradually move up the right side of your abdomen. Continue across just below your ribcage, then down the left side. Complete 5-10 full circles, maintaining that feather-light touch throughout.
You can also try gentle pumping motions. Place your hands on your lower abdomen and press very lightly, then release. This rhythmic pumping helps stimulate lymphatic movement in the deeper abdominal lymph nodes.
While self-lymphatic drainage can be wonderfully beneficial for maintenance and minor concerns, it’s not a substitute for professional treatment when dealing with medical conditions like lymphedema or post-surgical swelling. Always consult with your healthcare provider about whether these techniques are appropriate for your specific situation, and continue working with qualified therapists for comprehensive care.[15]
Tools and Devices for Lymphatic Drainage
Lymphatic drainage devices come in many forms, from simple brushes to advanced systems. They help support fluid flow in your body. You can find affordable tools for home use or medical-grade equipment that needs a doctor’s help.
Some tools are for general wellness, while others are part of medical treatment. It’s important to know the difference and choose tools that fit your health goals.
The Art and Science of Body Brushing
Dry brushing is a popular way to support lymphatic health and refresh your skin. It involves using a natural-bristle brush on dry skin before showering. This creates a gentle massage that many find invigorating.[17] Supporting gut health alongside your lymphatic system — for example through probiotics for gut and immune balance — creates a comprehensive wellness foundation.
To dry brush effectively, start at your feet and move upward using long, sweeping strokes toward your heart. Use circular motions on your joints and stomach. Always brush in the direction of lymph flow, from extremities to the trunk.

Dry brushing takes just five to ten minutes. Use light to medium pressure. You shouldn’t feel discomfort or see redness that lasts more than a few minutes.
Many people feel energized and notice smoother skin with regular practice. Choose a brush with natural bristles and a long handle. Replace your brush every six to twelve months as the bristles wear down.
Facial Tools for Targeted Support
Gua sha tools and facial rollers are specialized for the face and neck. These smooth instruments, often made from jade, rose quartz, or stainless steel, gently encourage lymph flow. Using them with light pressure may help reduce morning puffiness and promote a healthy glow.
Facial rollers have one or two smooth cylinders that glide across your skin. Roll from the center of your face outward and from your jawline up toward your temples. This directional movement supports the natural flow of lymphatic fluid toward drainage points in your neck.
Gua sha involves flat, sculpted stones that you sweep across your face at specific angles. The technique requires learning proper hand positioning and pressure. Many people enjoy incorporating these tools into their morning or evening skincare routines as a relaxing ritual.
Keep in mind that results from facial tools are temporary. They work best when combined with proper hydration, good sleep, and other healthy habits. Always use these tools on clean skin with a facial oil or serum to prevent tugging.
Medical-Grade Compression Solutions
Compression garments and pneumatic compression pumps are the medical side of lymphatic drainage devices. They play a key role in complete decongestive therapy for conditions like lymphedema. Unlike wellness tools, these devices require professional fitting and medical guidance to ensure safety and effectiveness.
Compression garments apply graduated pressure to prevent fluid accumulation and encourage lymphatic circulation. They come in various styles including sleeves, stockings, and full-body options. A trained specialist measures your limbs carefully to ensure proper fit, as incorrect sizing can worsen swelling or cause discomfort.
Pneumatic compression pumps are inflatable sleeves connected to a machine that applies rhythmic pressure to your limbs. This controlled compression mimics the natural muscle contractions that move lymph fluid. Healthcare providers typically prescribe these devices for home use as part of a comprehensive treatment plan.
The pressure settings and duration of compression therapy must be customized to your specific condition. Never use medical compression devices without consulting your healthcare provider first. When used correctly under professional supervision, these tools can significantly improve quality of life for people managing lymphatic challenges.
Whether you’re exploring simple dry brushing or need medical-grade compression therapy, the right tools can enhance your lymphatic support routine. Start with basic options for general wellness, and always seek professional advice for medical-grade lymphatic drainage devices.
Exercise and Movement for Lymphatic Health
Your lymphatic system needs movement to work right. Without it, fluid can get stuck in your tissues. But, you don’t need to do hard workouts to help it. Gentle, regular movement is what it likes best.
When you move, you’re actually helping your lymphatic system. This is because your muscles squeeze the lymphatic vessels. This action pushes fluid through your body, helping to remove waste and toxins.[7]
Think of moving as a way to help your body’s cleaning crew. Even a short walk can make a big difference in how well your lymphatic system works.
Low-Impact Activities That Boost Circulation
The best exercises for your lymphatic system are those that use big muscles but don’t hurt your joints. Walking is a great choice because it’s easy and effective. A brisk walk of 15 to 20 minutes can help your lymphatic system all over your body. Weaving lymphatic-supportive movement into building a balanced daily wellness routine amplifies long-term results.
Swimming is also very good because the water pressure helps move your lymph fluid. The swimming motions work many muscles at once. Plus, swimming helps move fluid that might be stuck in your legs.
Cycling is another good choice because it works your legs, which have a lot of lymphatic vessels. The pedaling motion helps move fluid through your body. Start with just 10 minutes and gradually build up as your stamina improves.
- Tai Chi and Qigong for gentle, flowing movements
- Pilates for controlled muscle engagement
- Water aerobics for lymphatic stimulation with joint protection
- Gentle stretching routines that promote flexibility
The Power of Bouncing Movements
Rebounding on a mini-trampoline is a great way to boost your lymphatic flow. The up-and-down motion helps move fluid through your body. Each bounce opens and closes the valves in your lymphatic vessels.
You don’t need to jump high to get benefits from rebounding. Even gentle bouncing can help. Just 10 to 15 minutes of rebounding can stimulate lymph circulation throughout your entire system.
If you don’t have a rebounder, jumping jacks or skipping rope can also help. The vertical movement and landing impact help move fluid. These activities create a pumping action in your body.
For those with joint concerns or balance issues, marching in place with high knee lifts is a gentler option. Lift your knees as high as you can while keeping your breathing steady.
Specific Poses for Enhanced Drainage
Yoga can help your lymphatic system by using gentle movements and stretches. Some poses target areas with lots of lymph nodes, helping to clear them out.
Legs-up-the-wall pose is especially good for your lymphatic health. Lie on your back with your legs up against a wall for 10 to 15 minutes. This pose helps drain fluid from your lower body.
Downward-facing dog is another good pose. It helps drain your legs and gently compresses your abdominal lymphatic vessels. The pose also encourages deep breathing, which helps move lymph fluid. Hold this pose for five to eight breaths, then rest and repeat.
Twisting poses like seated spinal twist and supine twist are also helpful. They gently compress your torso, helping to move lymph fluid. These poses are especially good for your abdominal lymphatics.
Child’s pose is a restorative pose that gently compresses your chest and abdomen. It promotes drainage from your head and neck while calming your nervous system.
| Exercise Type | Lymphatic Benefit | Recommended Duration | Best For |
|---|---|---|---|
| Walking | Full-body muscle contractions stimulate overall lymph flow | 15-30 minutes daily | Beginners and all fitness levels |
| Rebounding | Vertical motion activates lymphatic valves throughout body | 10-15 minutes, 3-5 times weekly | Those seeking efficient lymphatic stimulation |
| Swimming | Water pressure provides external compression while muscles pump internally | 20-30 minutes, 2-3 times weekly | Joint-friendly lymphatic support |
| Yoga inversions | Reverses gravity to drain accumulated fluid from lower body | 5-15 minutes daily | Reducing lower body swelling and congestion |
Consistency matters more than intensity when it comes to lymphatic health. Choose activities you enjoy so you’ll keep doing them. Your lymphatic system prefers regular, moderate movement over intense workouts.
Remember to breathe deeply while you exercise. Slow, deep breaths help your lymphatic system by creating pressure changes in your chest. This helps pull lymph fluid upward toward your heart.
Nutrition and Hydration for a Healthy Lymphatic System
What you eat and drink is key to a healthy body. The right lymphatic system nutrition helps remove waste and reduce inflammation. A good lymphatic diet focuses on adding good foods, not cutting out too much.
Your food choices affect how well lymph fluid moves. Eating nutrient-rich foods helps your lymphatic system work better.
Nutrient-Rich Foods That Boost Lymphatic Performance
Some foods are great for your lymphatic health. Anti-inflammatory foods are especially important. They help your drainage system work better.[8]
Leafy greens and cruciferous vegetables are must-haves. Spinach, kale, broccoli, and Brussels sprouts help detoxify your body. They also keep your lymphatic vessels strong.

Berries and fruits rich in antioxidants protect your lymphatic tissues. Blueberries, strawberries, and cherries boost your immune system. Citrus fruits add vitamin C and support lymph node functions.
Fish and flaxseeds are good for omega-3 fatty acids. These fats reduce inflammation and keep lymph fluid flowing. Wild-caught salmon, sardines, mackerel, and chia seeds are great sources. Exploring evidence-based nutritional support for your body’s lymphatic drainage system can complement dietary choices when additional lymphatic support is needed.
Nuts and seeds are full of healthy fats, protein, and minerals. Almonds, walnuts, pumpkin seeds, and sunflower seeds are great snacks. They give you energy and support your lymphatic health.
Herbs and spices like ginger and turmeric are anti-inflammatory. They add flavor and help your lymphatic system. Fresh garlic also supports your immune system.[20]
Eat at least two-thirds of your plate with vegetables, fruits, whole grains, nuts, and seeds. This way, you avoid bad foods and get lots of nutrients.
Water Intake: The Foundation of Lymph Flow
Drinking enough water is crucial for your lymphatic health. Your lymph fluid is mostly water. Not drinking enough can slow it down.
When you drink enough water, your lymph flows well. But dehydration makes it thick and hard to move. This can lead to waste buildup and fluid imbalance.
Most adults need eight to ten glasses of water a day. Start with a glass of water in the morning to help your lymphatic system.
Herbal teas like red clover, cleavers, and calendula support your lymphatic system. Green tea also adds antioxidants.
Carry a reusable water bottle to remind you to drink. Add lemon, cucumber, or mint for flavor. Drink water regularly for better absorption.
Dietary Choices That Compromise Lymphatic Function
Adding good foods is key, but knowing what to limit is also important. Some foods can harm your lymphatic system.
Too much sodium can make you retain water. Processed foods often have hidden sodium. Choose fresh foods instead.
Refined sugars and processed foods cause inflammation. They offer little nutrition and can make you gain weight. This puts extra strain on your lymphatic system.
Limit red meat and choose lean proteins like chicken, fish, and beans. Avoid processed meats like bacon and deli meats. They contain preservatives that cause inflammation.
Drinking too much alcohol dehydrates you and hurts your lymphatic system. Drink in moderation and drink more water. Keeping a healthy weight also helps your lymphatic system.
Being overweight or obese damages your lymphatic system and increases cancer risk. It causes inflammation and hormonal imbalances. Eating well and exercising helps protect your lymphatic vessels.
| Foods to Embrace | Primary Benefits | Foods to Limit | Why Reduce Them |
|---|---|---|---|
| Leafy greens and cruciferous vegetables | Detoxification support and vessel health | Processed meats | High sodium and inflammatory compounds |
| Berries and citrus fruits | Antioxidants and immune support | Refined sugars | Trigger inflammation and weight gain |
| Fatty fish and flaxseeds | Omega-3s reduce inflammation | Excessive alcohol | Causes dehydration and impaired function |
| Nuts and seeds | Healthy fats and minerals | High-sodium packaged foods | Promote fluid retention |
Remember, healthy eating for your lymphatic system is about progress, not perfection. Small changes can make a big difference over time. Focus on making positive choices for your lymphatic health.
Breathing Techniques and Their Impact on Lymphatic Flow
One of the most overlooked yet powerful ways to support lymphatic drainage costs nothing and is available to you every single moment of the day—your breath. The lymphatic system doesn’t have its own pump like the heart provides for blood circulation. Instead, it relies on physical activity like exercise and deep breathing exercises to move lymph fluid through your vessels and nodes.
When you practice proper breathing techniques, you create pressure changes in your chest and abdomen that act like a natural pump for your lymphatic system. This mechanical action is particularly effective at stimulating the largest lymphatic pathways running through your core.[16]
The beauty of lymphatic breathing techniques is their accessibility. You can practice them anywhere, anytime, without special equipment or training. Plus, you’ll enjoy immediate relaxation alongside the lymphatic support.
The Power of Belly Breathing
Diaphragmatic breathing, often called belly breathing, is the foundation of effective lymphatic support through breathwork. This technique focuses on engaging your diaphragm—the large muscle beneath your lungs—rather than shallow chest breathing.
When you practice diaphragmatic breathing correctly, the movement of your diaphragm creates rhythmic pressure changes that help pump lymph fluid through your system. This is especially powerful because it stimulates two critical structures: the thoracic duct and cisterna chyli, the largest lymphatic vessels in your body that run through your core.
Here’s how to practice proper diaphragmatic breathing:
- Sit or lie down in a comfortable position where you can fully relax
- Place both hands on your belly to feel the movement and ensure proper technique
- Breathe in slowly through your nose, focusing on expanding your belly as you inhale
- Your chest should remain relatively still while your abdomen rises
- Exhale slowly through your mouth, contracting your belly as you breathe out
- Feel your abdomen gently fall back toward your spine
Start with just five minutes of practice. As you become comfortable with the technique, you’ll notice it becomes more natural. The key is maintaining that belly expansion and contraction with each breath cycle.
Deep belly breathing is particularly effective for lymphatic health because that rhythmic motion helps lymph to flow through the central vessels of your body. Think of your diaphragm as a gentle massage tool working from the inside out.
Simple Breathing Exercises for Daily Practice
Once you’ve mastered basic diaphragmatic breathing, you can incorporate specific breathing exercises into your daily routine. These techniques amplify the deep breathing benefits while fitting easily into your schedule.
The 4-7-8 Breathing Technique is excellent for lymphatic flow and relaxation. Inhale through your nose for a count of four, hold your breath for seven counts, then exhale completely through your mouth for eight counts. This extended exhalation creates stronger pressure changes that enhance lymphatic movement.
Box breathing offers another powerful option. Breathe in for four counts, hold for four, exhale for four, and hold empty for four. This balanced pattern creates consistent, rhythmic pressure that supports steady lymphatic flow throughout the practice.
For maximum benefit, practice breathing exercises at these optimal times:
- Five minutes each morning upon waking to jumpstart lymphatic circulation
- Five minutes each evening before bed to support overnight detoxification
- Brief sessions during work breaks to maintain consistent lymphatic activity
- Before or after exercise to complement physical movement benefits
You can enhance your lymphatic breathing techniques by combining them with other supportive practices. Try pairing deep breathing with gentle self-massage, particularly around your neck and chest where major lymph nodes cluster. The combination provides synergistic benefits that neither practice delivers alone.
Some people find it helpful to practice breathing exercises while doing light stretching or while lying with legs elevated. These positions complement the breathing work by using gravity to assist lymphatic return.
The wonderful aspect of breathing exercises is their immediate accessibility. Unlike some wellness practices that require planning, equipment, or significant time investment, you can practice supportive breathing anywhere. Whether you’re sitting at your desk, lying in bed, or waiting in line, you have the opportunity to support your lymphatic system.
Remember that consistency matters more than duration. Even two minutes of focused diaphragmatic breathing three times daily provides meaningful support for your lymphatic system. As this becomes habit, you’ll likely notice you naturally breathe more deeply throughout your day, creating ongoing benefits without conscious effort.
Other Lifestyle Practices That Support Lymphatic Drainage
Exercise and manual techniques are key, but other lifestyle practices also help your lymphatic system. These simple habits work with massage and movement to improve drainage naturally. They’re easy to add to your daily routine without adding stress. At our evidence-based health resource center, you will find comprehensive guides on supporting every system in your body.
These practices are enjoyable and relaxing. They become part of a self-care routine, not extra work. Let’s look at some effective options for your lymphatic health.
Water Therapy and Temperature Contrast
Hydrotherapy has been used for centuries to promote health and healing. Contrast showers, alternating warm and cool water, are very effective. This temperature change helps your blood and lymphatic vessels expand and contract, promoting a natural pumping action.[10]
Start with warm water for three minutes. Then switch to cool water for 30 seconds to one minute. Repeat this cycle three to five times, ending with cool water.
The temperature contrast stimulates lymphatic flow and invigorates your system. Many people feel energized and refreshed after using contrast showers. Start with gentle temperature differences and increase the contrast as you get used to it.
Swimming is another great form of hydrotherapy. Moving through water provides built-in compression for your body, encouraging lymphatic drainage. The water’s gentle resistance also supports muscle contractions that help pump lymph fluid.
You don’t need to swim laps to benefit. Even gentle water walking or aquatic exercises can help your lymphatic function. The water’s pressure creates an ideal environment for fluid movement in your body.
Heat Exposure and Its Effects
Sauna therapy is known for its health benefits, including improved circulation and relaxation. Regular sauna use can promote overall wellness and help release toxins through sweating. The heat encourages blood flow and supports various bodily functions.
However, sauna benefits aren’t for everyone. If you have lymphedema or certain lymphatic conditions, heat can increase swelling. The warmth may cause blood vessels to dilate, leading to fluid accumulation in affected areas.
Before starting regular sauna sessions, talk to your healthcare provider if you have lymphatic concerns. They can determine if heat therapy is safe for you. For most healthy individuals, moderate sauna use can be a relaxing addition to wellness practices.
Rest, Recovery, and Relaxation
The connection between sleep and lymphatic health is significant. Quality sleep is when your body repairs and detoxifies. Recent research shows the brain’s lymphatic system, called the glymphatic system, is active during deep sleep.
During restful sleep, your body clears waste and maintains the lymphatic system. Aim for seven to nine hours of quality sleep each night. Create a consistent bedtime routine, keep your bedroom cool and dark, and limit screen time before bed to support healthy sleep patterns.
Chronic stress can lead to inflammation and fluid retention. When stressed, your nervous system stays in fight-or-flight mode, affecting lymphatic drainage. Research shows manual lymphatic drainage on the neck may slow the heart rate and reduce blood pressure in healthy individuals.
These reactions are signs of your body calming its nervous system and entering a relaxed state. Another study found lymphatic drainage on the abdomen may increase relaxation in people under psychological stress. This shows the important connection between relaxation and lymphatic function.
Effective stress management supports both lymphatic and overall health. Consider adding these relaxation techniques to your daily routine:
- Meditation or mindfulness practices for 10-15 minutes daily
- Gentle yoga that combines movement with deep breathing
- Progressive muscle relaxation exercises before bedtime
- Spending time in nature or engaging in enjoyable hobbies
- Limiting exposure to stressful news or social media
You don’t need to master every stress management technique at once. Start with one or two practices that appeal to you and build from there. Even small steps toward reducing stress can support your lymphatic system’s natural function while improving your quality of life.
Remember, these lifestyle practices work best when combined with other supportive habits like proper nutrition, hydration, and regular movement. They’re part of a comprehensive approach to lymphatic health. By making gradual changes and finding what works for your unique needs, you’ll create a sustainable routine that supports drainage naturally.
Lymphatic Drainage for Specific Conditions
Lymphatic drainage can be a key part of your treatment plan for specific health challenges. The techniques are similar, but the approach and goals change based on your condition. Condition-specific treatment focuses on meeting your unique needs.
This therapy helps manage different health concerns. Each condition gets targeted strategies that work with your medical care.
Managing Lymphedema with Specialized Care
Lymphedema treatment is a main use of manual lymphatic drainage. This condition causes swelling when your lymphatic system can’t drain fluid well.[22]
Cancer treatment is a common cause of lymphedema in the U.S. Radiation and lymph node removal can damage your lymphatic system. But, other conditions like rheumatoid arthritis and chronic venous insufficiency can also cause it. Whole-body detoxification approaches — including a guided parasite cleanse and full-body detoxification protocol — are sometimes incorporated as adjuncts to lymphatic therapy.
The best approach is Complete Decongestive Therapy (CDT). This lymphedema treatment includes:[18]
- Manual lymphatic drainage to improve fluid movement
- Compression bandages and garments to keep results
- Special skin care to prevent infections
- Therapeutic exercise to pump lymph fluid
- Patient education for self-care
Working with a certified lymphedema therapist is key. They’ll create a plan that fits your swelling patterns and lifestyle.
Supporting Recovery After Cosmetic Procedures
Post-surgery lymphatic drainage helps with cosmetic procedure recovery. Early studies show it reduces swelling, bruising, and healing time.
Cosmetic surgeons now recommend it for many procedures:
- Abdominal liposuction and body contouring
- Breast augmentation or reduction surgery
- Facelift and eyelid procedures
- Facial treatments including injectables and fillers
- Arm or thigh lift after weight loss
Patients often report better results with post-surgery lymphatic drainage. The massage helps clear surgical trauma and reduces fluid buildup.
Always check with your surgeon about the right timing. Most recommend starting sessions a few days to a week after surgery.
Finding Relief with Chronic Fatigue and Fibromyalgia
People with chronic fatigue and fibromyalgia face many symptoms. Lymphatic drainage isn’t a cure but may help reduce some discomfort.
The gentle massage of lymphatic drainage is appealing for those with pain sensitivity. It uses light pressure that won’t hurt tender points in fibromyalgia.
The relaxation response from lymphatic drainage may help manage stress and tension that worsen chronic conditions.
Some with chronic fatigue report less “brain fog” and better energy after sessions. Others see reduced swelling in hands and feet.
Be realistic with your healthcare provider. Lymphatic drainage works best as part of a broader management strategy.
Understanding Cellulite Reduction Results
Let’s be honest about cellulite reduction claims. Lymphatic drainage may temporarily improve cellulite appearance, but it doesn’t eliminate the structural causes.
Cellulite forms when fat cells push through connective tissue. Lymphatic drainage can reduce fluid retention, making your skin look smoother temporarily. It’s like reducing puffiness, not changing the structure.
For the best cellulite reduction results, combine lymphatic drainage with:
- Regular exercise to tone muscles
- Hydration for skin health
- A balanced diet
- Dry brushing or other circulation-boosting practices
Improvements usually last a few days to a week. To keep results, you need consistent sessions and lifestyle support.
Remember, cellulite is normal and affects most people. If you choose lymphatic drainage for appearance, do it for yourself, not for unrealistic beauty standards.
When to Avoid Lymphatic Drainage and Potential Side Effects
Lymphatic drainage is usually safe, but some health conditions make it unsafe. Knowing the risks helps you make smart choices for your health. It’s important to know when to avoid it to prevent serious problems.
This therapy boosts fluid flow in your body. While it’s good for most people, it can be risky for those with certain health issues.
Contraindications and Safety Concerns
Some health conditions mean you should not get lymphatic drainage. This is because it can move fluids and increase circulation in ways that might harm you.[2]
Active infections are a big concern. For example, cellulitis, a bacterial skin infection, can spread fast if fluid movement increases. This could make the infection worse.
Blood clots and deep vein thrombosis are also big no-nos. MLD can dislodge a clot, leading to serious problems like pulmonary embolism or stroke.
Heart and kidney conditions need extra care. If your heart can’t pump blood well, adding more fluid can be too much. Kidney failure means your body can’t filter fluids properly, making increased flow dangerous.
| Condition | Why to Avoid MLD | Risk Level |
|---|---|---|
| Active Infections (Cellulitis) | May spread bacteria to healthy tissues | High |
| Blood Clots/Deep Vein Thrombosis | Can dislodge clots causing stroke or embolism | Critical |
| Congestive Heart Failure | Overburdens compromised heart function | High |
| Kidney Failure | Kidneys cannot process increased fluid load | High |
| Malignant Tumors (without approval) | May facilitate cancer cell spread | Critical |
Malignant tumors are another concern. Unless your oncologist says it’s okay, avoid lymphatic drainage. It might help cancer cells spread through your body.
Recent stroke survivors should talk to their doctor before trying MLD. The therapy can stress recovering blood vessels in the brain.
Possible Temporary Reactions
Even when it’s safe, you might feel some side effects. These usually mean your body is reacting to the treatment and go away in a day or two.
Increased urination is common. Your kidneys work hard to get rid of the fluid your lymphatic system releases. You might need to go to the bathroom more often, especially after your first few sessions.
Mild fatigue can happen as your body gets rid of toxins and waste. This tiredness usually goes away with rest and drinking water.
Some people get slight headaches after treatment. This is because your body is adjusting to better circulation and getting rid of waste. Drinking water can help lessen this effect.
Temporary symptom increases can happen before you start feeling better. Your lymphedema might look worse for a day or two as fluid moves through congested areas. This is normal and means the drainage is working.
When to Consult a Healthcare Provider
Some groups should always talk to a doctor before starting lymphatic drainage. Taking these precautions helps keep you safe and ensures the treatment works well.
Anyone with existing medical conditions should get a doctor’s okay first. This includes diabetes, autoimmune disorders, chronic infections, or any ongoing health concerns. Your doctor can decide if lymphatic drainage is safe for you.
People on medications need to get advice from their doctor. Blood thinners, immunosuppressants, and certain other drugs might interact with lymphatic drainage. Your healthcare provider can check if there are any risks based on your medications.
Pregnant women should also talk to their obstetrician about lymphatic drainage. While some gentle techniques might be safe, getting professional advice ensures both mom and baby stay safe.
Unexplained swelling needs a doctor’s check-up before trying lymphatic drainage. Swelling might mean a serious condition that needs treatment, not just self-care.
If you notice unusual reactions during or after lymphatic drainage, call your healthcare provider right away. Warning signs include severe pain, increased swelling, fever, redness spreading from the treatment area, or trouble breathing. These symptoms need immediate medical help and should never be ignored.
Conclusion
This summary shows a key fact: if your lymphatic system is healthy, drainage massage won’t do much more than relax you. Your body works well on its own. The lymphatic system does its job well when everything is in balance.
Instead, focus on what really matters for your health. Regular exercise, balanced eating, and staying hydrated are key. These habits help your body work as it should. Getting enough sleep and managing stress are also crucial for your well-being.
But, for those with lymphedema, swelling after surgery, or certain health issues, manual lymphatic drainage can help. Trained therapists can offer significant relief when your lymphatic system needs it.
Be smart about health info. Knowing what really works and what doesn’t helps you make better choices. Social media often makes health topics seem simpler than they are.
Your lymphatic system is amazing at its job. Support it with healthy habits every day. Start with small, lasting changes. Drink plenty of water, exercise regularly, eat well, and sleep well.
If you have concerns about your lymphatic system, talk to your doctor. They can give advice tailored to you. Now, you have tools to improve your health starting today.
Frequently Asked Questions
What exactly is lymphatic drainage and why has it become so popular?▼
It’s not just a trend. There’s real science behind it, especially for those with lymphedema or recovering from surgery. For most, healthy habits like movement and hydration work just as well as treatments.
How do I know if my lymphatic system isn’t working properly?▼
Signs of poor lymphatic function include swelling, frequent infections, and slow healing. You might also feel tired, stiff, or have unexplained aches. Skin changes and feeling heavy in your limbs are other signs.
If you’re experiencing these symptoms, see a healthcare provider. They can check if your lymphatic system is the issue and suggest treatment.
Is manual lymphatic drainage the same as regular massage?▼
No, manual lymphatic drainage (MLD) is different from regular massage. MLD uses light, circular movements to gently stretch the skin. It’s so light, it only moves the skin surface.
MLD follows specific pathways and sequences. It starts by clearing central lymph node areas before moving fluid to these points. It requires special training and is surprisingly relaxing.
Can I do lymphatic drainage massage on myself at home?▼
Yes, you can do self-lymphatic drainage at home for wellness. But first, learn proper technique from a qualified therapist. Use light pressure and follow the direction of lymph flow.
Self-massage can help reduce puffiness and support lymphatic health. But it’s not a substitute for professional treatment for conditions like lymphedema.
What should I look for when choosing a lymphatic drainage therapist?▼
Look for therapists with specific lymphatic drainage training. Certified Lymphedema Therapists (CLTs) are especially qualified for lymphedema or medical concerns. Physical therapists or massage therapists with MLD certification are also good choices.
Ask about their training, experience, and technique. Your healthcare provider may also provide referrals to qualified therapists.
How often do I need professional lymphatic drainage treatments?▼
Treatment frequency varies based on your needs and goals. People with lymphedema might need sessions daily at first. For post-surgical recovery, you might need a few sessions over weeks.
For general wellness or mild puffiness, monthly or occasional sessions might be enough. Your therapist will create a personalized plan. Frequency often decreases as you progress.
Does dry brushing really help with lymphatic drainage?▼
Dry brushing may provide some lymphatic stimulation and exfoliation benefits. It involves brushing dry skin with a natural-bristle brush in long, sweeping motions toward your heart. While evidence is limited, it aligns with lymphatic principles.
Many people find it invigorating and report feeling less puffy or more energized. It’s a gentle way to exfoliate and increase body awareness.
What’s the best type of exercise for supporting lymphatic health?▼
The best exercise for lymphatic health is regular movement. Walking is excellent and accessible for most. Swimming and aquatic exercise are also beneficial because water pressure encourages drainage.
Rebounding (jumping on a mini-trampoline) is especially effective. Cycling, dancing, and activities that engage large muscle groups also support lymphatic flow. Gentle yoga can also encourage drainage through positioning and gentle compression.
Can lymphatic drainage help me lose weight or reduce cellulite?▼
Lymphatic drainage is not a weight loss treatment. It doesn’t burn fat or cause permanent weight reduction. It can temporarily reduce fluid retention and bloating, making you look and feel less puffy.
Regarding cellulite, lymphatic drainage might temporarily improve its appearance by reducing fluid retention. However, these effects are temporary and don’t address the structural causes of cellulite. For sustainable weight management and body composition changes, focus on balanced nutrition, regular exercise, adequate sleep, and stress management.
Is lymphatic drainage safe during pregnancy?▼
Pregnancy causes significant changes in fluid balance and circulation. Many pregnant women experience swelling, particularly in the legs and feet during the second and third trimesters. While gentle lymphatic drainage techniques may help reduce swelling, it’s essential to consult with your healthcare provider before beginning any lymphatic drainage treatments during pregnancy.
Some techniques and areas should be avoided during pregnancy, and certain contraindications may apply. If your doctor approves, work only with therapists experienced in prenatal lymphatic drainage who understand the specific modifications needed during pregnancy. Gentle self-care approaches like elevating your legs, staying hydrated, walking regularly, and wearing appropriate compression stockings (if recommended by your provider) are generally safe ways to support lymphatic health during pregnancy.
When should I absolutely avoid lymphatic drainage?▼
There are several important contraindications where lymphatic drainage should not be performed. Avoid lymphatic drainage if you have active infections (especially cellulitis or skin infections), blood clots or deep vein thrombosis, congestive heart failure, kidney failure, acute inflammation, or untreated cancer.
If you’ve had a recent stroke, have uncontrolled high blood pressure, or have certain heart conditions, lymphatic drainage may not be safe. The reasoning is that MLD increases fluid circulation throughout the body, which in these conditions could spread infection, dislodge blood clots, or overburden organs that are already struggling. If you have any medical conditions or take medications, always consult your healthcare provider before beginning lymphatic drainage treatments. This is a therapeutic technique with real physiological effects, not just a relaxing spa treatment.
What should I eat to support my lymphatic system?▼
A diet that supports lymphatic health focuses on nutrient-dense, anti-inflammatory foods. Prioritize leafy greens and cruciferous vegetables like spinach, kale, broccoli, and Brussels sprouts, which contain antioxidants and nutrients that support detoxification. Berries and other colorful fruits provide antioxidants that protect lymphatic vessels.
Omega-3 fatty acids from fish (like salmon and sardines), flaxseeds, and walnuts help reduce inflammation. Nuts, seeds, herbs, and spices—particularly ginger, turmeric, and garlic—also support lymphatic and immune function. Adequate hydration is absolutely crucial since lymph fluid is primarily water. On the other hand, limit excessive sodium (which promotes fluid retention), processed foods, refined sugars, and excessive alcohol. Maintaining a healthy weight through balanced nutrition is also important, as obesity can damage the lymphatic system and increase lymphedema risk.
How long does it take to see results from lymphatic drainage?▼
The timeline for seeing results varies significantly depending on what you’re addressing and your individual circumstances. For temporary puffiness or mild swelling, you might notice improvement immediately after a professional session or even after self-massage—reduced facial puffiness, for example, can be visible within an hour. For post-surgical swelling, you might see gradual improvement over several sessions spanning weeks.
If you’re managing lymphedema, initial reduction in swelling typically occurs over the first few weeks of intensive treatment, but complete decongestive therapy is an ongoing process that requires consistent maintenance. For general wellness benefits like improved energy or better immune function, changes might be more subtle and develop over weeks or months of consistent practice. Remember that lymphatic drainage works best as part of a comprehensive approach that includes movement, proper nutrition, hydration, and other healthy lifestyle habits.
Can breathing exercises really help with lymphatic drainage?▼
Yes, proper breathing—particularly deep diaphragmatic breathing—is actually one of the most powerful and underutilized tools for supporting lymphatic drainage. When you breathe deeply using your diaphragm (so your belly expands rather than just your chest), the movement creates pressure changes in your chest and abdomen that act like a pump for your lymphatic system. This is especially effective because it stimulates the thoracic duct and cisterna chyli, which are the largest lymphatic vessels running through your body’s core.
Deep breathing provides immediate benefits—it’s free, you can do it anywhere, and it also promotes relaxation and stress reduction. Try spending just five minutes in the morning and evening practicing diaphragmatic breathing: breathe in slowly through your nose while letting your belly expand, then exhale through your mouth while your belly contracts. You can also incorporate deep breathing into movement, yoga, or self-massage for enhanced benefits.
Will insurance cover lymphatic drainage treatments?▼
Insurance coverage for lymphatic drainage varies significantly depending on your insurance plan, the reason for treatment, and who provides the service. Medical necessity is the key factor. If you have lymphedema—especially secondary lymphedema following cancer treatment—and the therapy is prescribed by a physician and performed by a certified lymphedema therapist or physical therapist, insurance is more likely to provide coverage.
Complete decongestive therapy for diagnosed lymphedema is often covered because it’s recognized as the standard medical treatment. However, lymphatic drainage for general wellness, cosmetic purposes, or minor puffiness is typically not covered and would be an out-of-pocket expense. Before beginning treatment, contact your insurance provider to ask specifically about coverage for manual lymphatic drainage, provide them with your diagnosis codes if applicable, and ask about prior authorization requirements, number of covered sessions, and any documentation needed from your healthcare provider.
Are facial lymphatic drainage tools like gua sha and jade rollers worth it?▼
Facial lymphatic drainage tools like gua sha stones and jade or rose quartz rollers have become incredibly popular. They can provide some benefits, though it’s important to have realistic expectations. When used with proper technique—gentle pressure, working in the direction of lymphatic flow (generally from the center of the face outward and downward toward the neck)—these tools can help reduce facial puffiness, particularly in the morning, and promote a temporary healthy glow.
The cool temperature of stone tools can also feel soothing and may help constrict blood vessels slightly, reducing redness. However, the results are typically temporary, lasting a few hours to perhaps a day. These tools won’t permanently change your facial structure, eliminate wrinkles, or provide dramatic long-term transformation. They’re best viewed as pleasant self-care rituals that provide modest, temporary benefits. If you enjoy using them and find the ritual relaxing, they can be a nice addition to your routine—just don’t expect miracle results.
What’s the difference between lymphatic drainage and a detox cleanse?▼
This is an important distinction. The lymphatic system performs genuine, scientifically-validated detoxification by physically collecting and removing cellular waste, bacteria, viruses, and other unwanted materials from your tissues and transporting them to organs that eliminate them from your body. This is real, measurable detoxification that happens continuously in your body.
In contrast, many commercial “detox cleanses” or “detox diets” make exaggerated claims that aren’t well-supported by science. Your body already has sophisticated detoxification systems—primarily your liver, kidneys, lymphatic system, and digestive system—that work continuously without special cleanses. Supporting lymphatic drainage through healthy lifestyle practices, proper hydration, movement, and nutrition helps your body’s natural detoxification systems work optimally. This is quite different from restrictive juice cleanses or expensive detox supplements that promise to remove mysterious “toxins”—your lymphatic system and other organs are already doing that work when you support them with fundamentally healthy habits.
Can I do lymphatic drainage if I have cancer or have had cancer treatment?▼
This requires careful individualized guidance from your oncology team. Historically, there was concern that lymphatic drainage might spread cancer cells through the lymphatic system, leading to a blanket contraindication for people with cancer. However, current understanding is more nuanced. For people with active, untreated cancer, lymphatic drainage is still generally contraindicated.
However, for cancer survivors, particularly those who developed lymphedema following surgery, radiation, or lymph node removal, manual lymphatic drainage is actually the cornerstone of treatment and is considered safe and beneficial. Many cancer centers now include certified lymphedema therapists as part of their supportive care teams. The key is working with therapists who have specific training in oncology and lymphedema, following protocols approved by your oncologist, and having open communication between your entire care team. Never begin lymphatic drainage without explicit approval from your cancer care providers.
Why do I need to urinate more after lymphatic drainage?▼
Increased urination after lymphatic drainage is actually a positive sign that the treatment is working. During manual lymphatic drainage, the therapist helps move stagnant fluid that has accumulated in your tissues back into circulation. This fluid then needs to be processed and eliminated by your body, which happens primarily through your kidneys and urinary system.
The increased urination means your body is successfully removing the mobilized fluid and the waste products it contains. This is a desired outcome, not a side effect to worry about. You might also notice that your urine is slightly darker or has a stronger odor temporarily, which reflects the concentrated waste products being eliminated. To support this process, make sure you’re drinking plenty of water before and after lymphatic drainage sessions. Staying well-hydrated actually helps your body eliminate the mobilized waste more efficiently and prevents you from feeling dehydrated despite the increased urination.
How is lymphedema different from regular swelling?▼
Lymphedema is a specific chronic condition where protein-rich fluid accumulates in tissues due to a damaged or compromised lymphatic system, causing progressive swelling that doesn’t resolve on its own. It’s different from temporary swelling you might experience from a twisted ankle, long flight, or eating salty foods. Regular swelling (edema) is often temporary and resolves when the underlying cause is addressed—elevate your ankle, the swelling goes down; reduce sodium, the puffiness decreases.
Lymphedema, however, is persistent and progressive without proper treatment. It most commonly develops following cancer treatment that involved lymph node removal or radiation, but can also result from infections, trauma, congenital conditions, or other causes. The swelling typically doesn’t improve with elevation alone, may feel heavy or tight, and the affected skin may develop a thickened, fibrotic quality over time. If you notice persistent, unexplained swelling that doesn’t improve with typical measures, consult a healthcare provider for proper evaluation. Early diagnosis and treatment of lymphedema significantly improves outcomes and quality of life.
Related Reading
Sources
- National Cancer Institute — Lymphedema (PDQ)
- Mayo Clinic — Lymphedema: Symptoms and Causes
- Cleveland Clinic — Lymphatic System Overview
- PubMed — Manual Lymphatic Drainage in Lymphedema Treatment
- PubMed — Complete Decongestive Therapy for Lymphedema
- PubMed — Lymphatic System and Immune Function
- PubMed — Exercise and Lymphatic Flow
- PubMed — Dietary Factors and Lymphedema Management
- Remedy’s Nutrition — Unlocking the Body’s Drainage System: Lymph Cleanse
- NIH NHLBI — Lymphatic Diseases
- Harvard Health — Understanding the Immune System
- WebMD — Lymphatic Drainage Massage
- Healthline — Lymphatic Drainage Massage: Benefits and How It Works
- Medical News Today — Lymphatic Drainage Massage
- American Cancer Society — Lymphedema
- PubMed — Lymphedema After Breast Cancer Treatment
- PubMed — Deep Breathing and Lymphatic Flow
- PubMed — Skin Microcirculation and Mechanical Stimulation
- Johns Hopkins Medicine — Lymphedema
- NCCIH — Massage Therapy for Health
- PubMed — Anti-inflammatory Diet and Lymphatic Health
- PubMed — Compression Therapy in Lymphedema
- Lymphatic Education and Research Network